Thyroglobulin Test Purpose, Procedure, Result and more
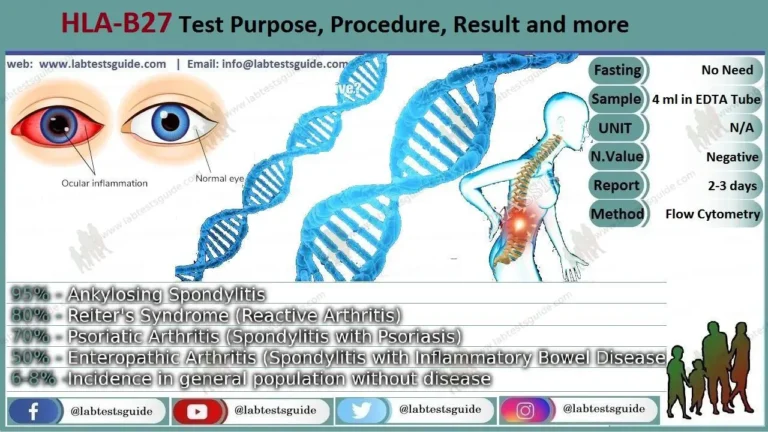
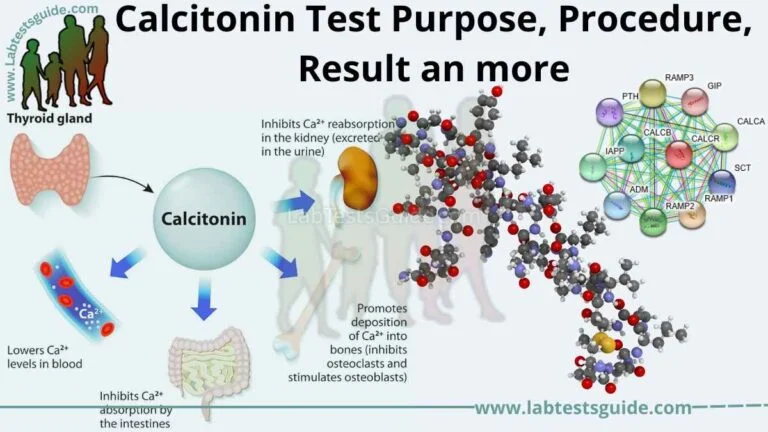
Thyroglobulin test measures the thyroglobulin level in the blood. Thyoglobulin is a cell -made protein. The thyroid is a small butterfly -shaped gland located near the throat. A thyoglobulin test is mainly used as a tumor marker test to help guide thyroid cancer.

Understand Your Test Results:
Understand your Thyroglobulin Test Results
AI-powered Lab Test Results Meaning tool 🤖
A glycoprotein hormone that is synthesized by the thyroid follicular cell and is incorporated by peptide bonds, with thyroid hormones (T3 and T4). The liberation of thyroid hormone occurs when T3 and T4 are enzymeatically divided from thyoglobulin. Tyroglobulin levels serve as a tumor marker to monitor the state of differentiated thyroid carcinomas.
| Also Known as | Tg, Thyroglobulin Tumor Marker, Thyroglobulin, Serum Thyroglobulin Test |
| Test Purpose | This test measures the thyroglobulin level in the blood |
| Test Preparations | At Least 6 Weeks Should Elapse After Thyroidectomy Or Needle Biopsy Or Iodine-131 Therapy Before Specimen Collection. |
| Test Components | Thyroglobulin (TG) |
| Specimen | 2 ML (1 ML Min.) Serum From 1 SST. |
| Stability Room | N/A |
| Stability Refrigerated | 48 Hours |
| Stability Frozen | 4 Weeks |
| Method | Chemiluminescent Immunoassay (CLIA) |
| Download Report | Download Report |
Thyoglobulin vs. Thyroglobulin antibody
Tyroglobulin tests measure TG protein in the bloodstream. Tyoglobulin antibody tests detect TG antibodies produced by the immune system and can cause thyroid damage.
Thyroid antibodies can influence the precision of the results of the TG test, which makes it harder to find a recurrence of cancer. Doctors order TG and TGAB tests by measuring thyroglobulin levels to verify if there is recurrence of thyroid cancer.
Why Get Tested:
A thyroglobulin test is mostly used to:
- See if thyroid cancer treatment was successful. If thyroglobulin levels stay the same or increase after treatment, it may mean there are still thyroid cancer cells in the body. If thyroglobulin levels decrease or disappear after treatment, it may mean there are no normal or cancerous thyroid cells left in the body.
- See if cancer has returned after successful treatment.
When to Get Tested:
- Doctors generally order the thyoglobulin test after thyroid cancer surgery, more frequently in combination with a neck ultrasound. It helps determine if cancer has returned.
- Detectable thyroglobulin levels that continue to increase one year after surgery suggest that cancer has returned. An ultrasound of the neck helps to confirm this.
- If the levels are undetectable within a year after surgery, the risk of return of cancer is low. However, if he had thyroid cancer, his levels will be monitored annually for life to make sure that he is not yet cancer free.
- Tyroglobulin antibodies (TGAB) can interfere with thug -globulin measurement and cause falsely low or undetectable levels. That is why a TGAB test is always ordered at the same time as a thyroglobulin test.
Sample required?
- A blood sample drawn from a vein in your arm
- 2 ML (1 ML Min.) Serum From 1 SST.
Test preparation needed?
At Least 6 Weeks Should Elapse After Thyroidectomy Or Needle Biopsy Or Iodine Therapy Before Specimen Collection.
Normal Values:
Source 1
- 0-11 months:
- Male – 0.6-5.5 ng/mL
- Female – 0.5-5.5 ng/mL
- 1-11 years:
- Male – 0.6-50.1 ng/mL
- Female – 0.5-52.1 ng/mL
- 12 years and older:
- Male – 0.5-53.0 ng/mL
- Female – 0.5-43.0 ng/mL
Source 2
- Male 1.40 – 29.2 ng/mL
- Female : 1.50 – 38.5 ng/mL
High Thyroglobulin Level is seen in :
- Thyroid Cancer
- Benign Thyroid Tumors
- Thyroid Nodules
- Underactive Thyroid
- Graves’ Disease
- Iodine Deficiency and Excess
- Liver Cirrhosis
- Acromegaly
- Medications
Low Thyroglobulin Level is seen in :
- Too many synthetic hormones T4
- Thyroid elimination
- Medicines
- Levothyroxin (synthroid)
- Synthetic TSH (Bitogen)
- Octreotid (saustatin), a somatostatin synthetic hormone
- Salicylate (aspirin)
- Prednisolone (omnipred), an anti -inflammatory corticosteroid
Understand Your Test Results:
Understand your Thyroglobulin Test Results
AI-powered Lab Test Results Meaning tool 🤖