Chorionic Villus Sampling (CVS) is a prenatal diagnostic procedure used to obtain a small sample of placental tissue from the developing embryo. This tissue, known as chorionic villi, contains genetic information that can be analyzed to assess the health and genetic makeup of the fetus. CVS is typically performed between the 10th and 13th weeks of pregnancy, earlier than other prenatal diagnostic procedures like amniocentesis.
Definition of CVS.
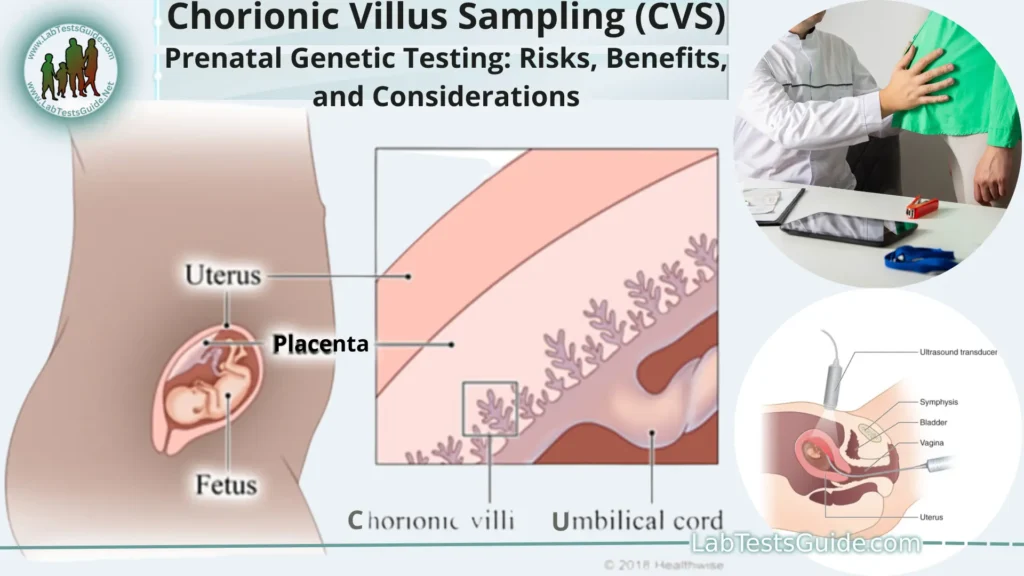
Chorionic Villus Sampling (CVS) is a medical procedure conducted during pregnancy to obtain a small sample of tissue from the chorionic villi, which are tiny finger-like projections found on the placenta. The chorionic villi contain genetic material that is representative of the developing fetus. This tissue sample is collected for diagnostic purposes to assess the genetic health of the fetus, detect chromosomal abnormalities, and identify certain genetic disorders. CVS is usually performed in the early stages of pregnancy and can provide valuable information to expectant parents and healthcare providers about the well-being of the fetus.
What is the Importance of Prenatal Genetic Testing?
- Detection of Genetic Abnormalities: Prenatal genetic testing allows for the early detection of genetic abnormalities, such as chromosomal disorders (e.g., Down syndrome, Edwards syndrome, Patau syndrome) and other genetic conditions. This early diagnosis enables parents to prepare for potential challenges and make informed decisions about the pregnancy and the care needed for the child after birth.
- Informed Decision-Making: Prenatal genetic testing provides parents with critical information that helps them make informed decisions about the continuation of the pregnancy, medical interventions, and planning for the child’s future. Understanding the potential risks and challenges allows parents to weigh their options and make choices that align with their values and circumstances.
- Medical Management and Care Planning: When certain genetic conditions or health concerns are identified prenatally, healthcare providers can develop appropriate medical management plans. This may involve specialized monitoring during pregnancy, consultations with pediatric specialists, and preparation for any necessary medical interventions after birth.
- Emotional and Psychological Preparation: Prenatal genetic testing allows parents to emotionally and psychologically prepare for the birth of a child with specific medical needs or conditions. Knowing in advance about potential challenges can help reduce feelings of shock or unpreparedness after birth.
- Family Planning and Reproductive Choices: Prenatal genetic testing results can influence future family planning decisions. If a genetic disorder is identified in one pregnancy, parents may choose to undergo genetic counseling and testing in subsequent pregnancies to assess the risk and explore options.
- Research and Advances in Treatment: Data collected through prenatal genetic testing contribute to medical research and the advancement of knowledge about genetic conditions. This research can lead to improvements in diagnostic techniques, treatments, and interventions for affected individuals.
- Ethical and Moral Considerations: Prenatal genetic testing raises important ethical questions about reproductive choices, autonomy, and the value of life. These considerations vary among individuals, families, and cultures, highlighting the complexity of decision-making in this context.
- Support and Resources: Prenatal genetic testing often opens the door to a network of support, including genetic counselors, medical professionals, and patient advocacy groups. These resources can provide emotional support, accurate information, and guidance throughout the journey.
Methods of Chorionic Villus Sampling:
Transcervical CVS:
Procedure: In this method, a thin catheter is inserted through the cervix (the opening of the uterus) under the guidance of ultrasound imaging. The catheter is threaded through the cervix and into the placental tissue, where a small sample of chorionic villi is aspirated.
Advantages: Transcervical CVS is a minimally invasive procedure that doesn’t require penetrating the abdominal wall. It’s generally quicker and may be associated with less discomfort.
Considerations: This method might be more suitable for pregnancies with a favorable cervix and proper positioning of the placenta. However, it might be more challenging in cases of certain cervical or uterine abnormalities.
Transabdominal CVS:
- Procedure: In this method, a thin needle is inserted through the abdominal wall and guided into the uterus using ultrasound imaging. The needle is then directed to the placenta, where a small sample of chorionic villi is collected.
- Advantages: Transabdominal CVS is suitable for a wider range of pregnancies, as it doesn’t depend on cervical factors. It’s often used when the placenta is positioned in a way that makes transcervical access difficult.
- Considerations: While still minimally invasive, transabdominal CVS involves penetrating the abdominal wall, which might cause mild discomfort. It’s important to ensure proper ultrasound guidance to avoid potential risks.
Timing and Eligibility:
Timing:
- CVS is usually performed between the 10th and 13th weeks of pregnancy, counting from the first day of the last menstrual period. This timeframe is chosen because the placental tissue contains sufficient genetic material for testing, and it allows for early detection of genetic abnormalities.
Eligibility:
- Advanced Maternal Age: Pregnant individuals who are 35 years or older at the time of delivery are often considered at higher risk for chromosomal abnormalities, such as Down syndrome. As such, they might be candidates for CVS.
- Previous Child with Genetic Condition: If a previous child was born with a genetic disorder, the parents might consider CVS to assess the genetic health of the current pregnancy.
- Positive Screening Tests: Abnormal results from non-invasive prenatal screening tests (NIPT) or other first-trimester screenings might lead to a recommendation for CVS to confirm or rule out genetic abnormalities.
- Family History: Families with a history of specific genetic disorders might be eligible for CVS to determine if the fetus is at risk of inheriting those disorders.
- Parental Carriers: If both parents are known carriers of a genetic disorder, CVS can help determine if the fetus has inherited the disorder.
- Parental Anxieties: In some cases, parents might request CVS due to personal or familial anxieties about genetic conditions, even in the absence of specific risk factors.
- Prior Pregnancy Losses: Individuals who have experienced multiple miscarriages or stillbirths might undergo CVS to investigate potential genetic factors contributing to these losses.
Procedure and Process:
- Pre-Procedure Preparation: Before the procedure, you will likely have a consultation with your healthcare provider or a genetic counselor to discuss the reasons for considering CVS, the potential risks and benefits, and any questions or concerns you may have.
If you decide to proceed with CVS, you might have an ultrasound to confirm the gestational age, determine the position of the placenta, and assess other relevant factors. - Ultrasound Guidance: On the day of the procedure, you will undergo an ultrasound to guide the healthcare provider in locating the placenta and determining the best approach for accessing it.
- Transcervical CVS: If the transcervical method is chosen and the cervix is favorable, a thin catheter will be inserted through the cervix under ultrasound guidance. The catheter is guided to the placenta, and a small sample of chorionic villi is aspirated.
Local anesthesia might be used to numb the cervix before the procedure. - Transabdominal CVS: If the transabdominal method is chosen or if cervix-related factors make the transcervical method less suitable, a thin needle will be inserted through the abdominal wall and guided into the uterus under ultrasound imaging.
The needle is directed to the placenta, and a small sample of chorionic villi is collected through the needle. - Sample Collection: The collected chorionic villi are then sent to a laboratory for genetic analysis. The genetic material is extracted from the sample for testing.
The laboratory will perform various tests, such as chromosomal analysis, to assess the genetic health of the fetus. - Post-Procedure Care: After the procedure, you might be observed for a short time to ensure there are no immediate complications.
It’s common to experience mild cramping and spotting after the procedure. These symptoms usually resolve on their own. - Genetic Counseling and Test Results: Once the genetic analysis is complete, you will have a follow-up appointment with your healthcare provider or genetic counselor to discuss the results.
The results will provide information about the presence or absence of specific genetic conditions or chromosomal abnormalities in the fetus.
Types of Genetic Testing with CVS:
Here are the main types of genetic testing that can be performed using CVS samples.
Chromosomal Analysis (Karyotyping):
- One of the primary purposes of CVS is to perform chromosomal analysis. This involves examining the number and structure of the chromosomes in the fetal cells.
- Chromosomal analysis can detect numerical abnormalities (aneuploidies), such as Down syndrome (trisomy 21), Edwards syndrome (trisomy 18), and Patau syndrome (trisomy 13).
- It can also identify structural chromosomal abnormalities, like translocations, deletions, and duplications.
- Fluorescence In Situ Hybridization (FISH): FISH is a technique used to detect specific chromosomal abnormalities associated with certain genetic disorders.
FISH can provide rapid results for a limited number of chromosomal abnormalities, such as Down syndrome, without the need for complete karyotyping. - Microarray Analysis (Chromosomal Microarray): Microarray analysis involves examining the entire genome for small gains or losses of genetic material, known as copy number variations (CNVs).
It can detect a wider range of chromosomal abnormalities and genetic syndromes caused by CNVs, providing more detailed information compared to traditional karyotyping. - Single Gene Disorder Testing: CVS can be used to test for specific single gene disorders if the parents are carriers or if there’s a known family history of a genetic condition.
This type of testing focuses on identifying mutations or changes in individual genes associated with particular genetic disorders. - Polymerase Chain Reaction (PCR) Testing: PCR is a molecular technique used to amplify specific segments of DNA for analysis.
It can be used to identify mutations in specific genes, such as those associated with genetic diseases like cystic fibrosis or sickle cell disease.
Risks and Considerations:
Here are the main risks and considerations associated with CVS.
- Miscarriage Risk: One of the primary risks associated with CVS is the risk of miscarriage. While the risk is relatively low (around 0.5% to 1%), it’s important to consider this potential outcome.
The risk might be slightly higher than with other prenatal tests, such as amniocentesis, which is typically performed later in pregnancy. - Procedure-related Discomfort: The procedure can cause mild discomfort, such as cramping or abdominal discomfort, during and after the procedure. This discomfort usually subsides within a short time.
- Procedure-related Complications: In rare cases, CVS can lead to complications such as infection, bleeding, or injury to the fetus or surrounding tissues. Properly performed under ultrasound guidance, the risk of such complications is minimized.
- Limited Genetic Information: While CVS provides valuable genetic information, it might not cover all possible genetic conditions. Some genetic disorders might not be detectable through CVS, and false-positive or false-negative results can occur.
- Emotional and Psychological Impact: The decision to undergo CVS and receive genetic test results can have emotional and psychological implications for expectant parents. Negative results can lead to relief, while positive results might lead to stress and difficult decisions.
- Ethical and Moral Considerations: Genetic testing can raise ethical questions about reproductive choices, parental responsibilities, and the value of life. These considerations can vary based on individual beliefs and cultural backgrounds.
- Alternative Testing Options: There are alternative prenatal testing options, such as non-invasive prenatal testing (NIPT) and amniocentesis, that might have different risk profiles and offer similar or complementary information.
- Results Interpretation: Genetic test results might not always be straightforward to interpret. Some results could indicate uncertain outcomes or variants of uncertain significance, which might require further testing or monitoring.
- Timeframe for Results: The timeframe for receiving results can vary. Some initial results might be available relatively quickly, but more comprehensive genetic testing might take longer to provide conclusive information.
Indications for Chorionic Villus Sampling:
Here are some common indications for undergoing CVS.
- Advanced Maternal Age: Pregnant individuals who are 35 years or older at the time of delivery are considered to have an increased risk of having a child with chromosomal abnormalities, such as Down syndrome (trisomy 21). CVS can be offered to assess the genetic health of the fetus in such cases.
- Positive Screening Tests: Abnormal results from non-invasive prenatal screening tests (NIPT) or other first-trimester screening tests might indicate an increased risk of genetic abnormalities. CVS can provide more definitive information about the genetic status of the fetus.
- Previous Child with Genetic Condition: If a previous child was born with a genetic disorder, there might be concerns about the recurrence of the condition in a subsequent pregnancy. CVS can be used to assess the genetic health of the current pregnancy.
- Family History of Genetic Disorders: Families with a history of certain genetic disorders might be at higher risk of having a child with the same condition. CVS can help determine whether the fetus has inherited the genetic condition.
- Parental Carriers of Genetic Disorders: If both parents are carriers of a specific genetic disorder (autosomal recessive conditions), there’s a chance the fetus could inherit the disorder. CVS can be used to test for the presence of the disorder in the fetus.
- Known Chromosomal Abnormalities in a Parent: If one of the parents carries a chromosomal abnormality, such as a balanced translocation, there’s an increased risk of having a child with unbalanced chromosomal rearrangements. CVS can provide information about the fetus’s chromosomal makeup.
- Prior Pregnancy Losses or Stillbirths: Individuals who have experienced multiple miscarriages or stillbirths might undergo CVS to investigate potential genetic factors contributing to these losses.
- Parental Anxieties or Concerns: Some parents might request CVS due to personal or familial anxieties about genetic conditions, even in the absence of specific risk factors.
Decision-Making and Informed Consent:
- Gathering Information: Begin by gathering information about CVS, its purpose, the procedure itself, the potential risks and benefits, and the conditions it can detect. This information can come from healthcare providers, genetic counselors, reliable medical sources, and educational materials.
- Consulting Healthcare Providers: Schedule appointments with your obstetrician, genetic counselor, or other healthcare providers who specialize in prenatal care and genetic testing. They can assess your medical history, family history, and other risk factors to help you make an informed decision.
- Understanding Your Risk Factors: Discuss your individual risk factors for genetic abnormalities with your healthcare provider. This includes considerations such as advanced maternal age, family history, previous pregnancies, and any existing genetic conditions.
- Balancing Risks and Benefits: Your healthcare provider will guide you in understanding the potential risks and benefits of CVS, as well as the alternatives. They can help you weigh the benefits of obtaining genetic information against the risks associated with the procedure.
- Genetic Counseling: Genetic counseling is a crucial step in the decision-making process. A genetic counselor can provide personalized information, answer your questions, and help you understand how the results of CVS might impact your family’s future.
- Considering Personal Values: Reflect on your personal values, beliefs, and priorities. Consider how the information obtained from CVS might influence your decisions and choices regarding the pregnancy, medical care, and family planning.
- Discussing with Partner: If applicable, involve your partner in the decision-making process. Both partners should have an opportunity to express their concerns, preferences, and opinions.
- Informed Consent: Informed consent is a formal process where you receive detailed information about the procedure, its risks, benefits, and alternatives. You have the opportunity to ask questions and clarify any uncertainties before providing your consent to undergo CVS.
- Documentation: After discussing the procedure and understanding its implications, you’ll be asked to sign an informed consent form. This document acknowledges that you have been fully informed about the procedure and have given your voluntary consent.
- Reviewing Your Decision: Take your time to review the information provided, the discussions you’ve had, and your own feelings about the procedure. If you’re uncertain or have more questions, don’t hesitate to seek additional information or counseling.
- Finalizing Your Decision: Once you’re confident in your decision, inform your healthcare provider about your choice. If you decide to undergo CVS, they will schedule the procedure and guide you through the necessary preparations.
Alternatives to CVS:
Here are some common alternatives.
- Amniocentesis: Amniocentesis is a procedure performed later in pregnancy, typically between the 15th and 20th weeks. It involves removing a small amount of amniotic fluid from around the fetus for genetic testing.
Like CVS, amniocentesis can provide information about chromosomal abnormalities and genetic disorders. It carries a lower risk of miscarriage compared to CVS but is performed later in pregnancy. - Non-Invasive Prenatal Testing (NIPT): NIPT is a blood test that analyzes cell-free fetal DNA present in the mother’s bloodstream. It’s typically performed around 10 weeks of pregnancy or later.
NIPT can screen for common chromosomal abnormalities such as Down syndrome, Edwards syndrome, and Patau syndrome, as well as certain sex chromosome abnormalities. - Ultrasound Screening: Ultrasound scans are routinely performed during pregnancy to monitor the growth and development of the fetus. Certain abnormalities, such as neural tube defects, can sometimes be detected through ultrasound.
- Carrier Screening: Carrier screening involves testing parents to determine if they carry gene mutations associated with certain genetic disorders. This information can help assess the risk of passing on these disorders to the child.
- Preimplantation Genetic Testing (PGT): PGT is a procedure used during in vitro fertilization (IVF) to test embryos for genetic abnormalities before they are implanted in the uterus. This can help select embryos without specific genetic conditions.
- Clinical Evaluation and Monitoring: In some cases, especially when specific genetic conditions aren’t suspected, healthcare providers may recommend close clinical evaluation, regular ultrasounds, and other monitoring throughout the pregnancy.
After CVS: Test Results and Follow-Up:
- Waiting for Results: The time it takes to receive your test results can vary depending on the specific tests performed and the laboratory’s processing times. Your healthcare provider will give you an estimate of when you can expect to receive the results.
- Follow-Up Appointment: Once the results are available, you will be scheduled for a follow-up appointment to discuss the findings. This appointment may be in person, over the phone, or through a secure online platform, depending on your healthcare provider’s practices.
- Results Interpretation: During the follow-up appointment, your healthcare provider or genetic counselor will explain the test results to you in detail. They will discuss whether any genetic abnormalities were detected and what those findings mean for your pregnancy.
- Understanding Implications: The healthcare provider will help you understand the implications of the results, potential next steps, and available options. If a genetic disorder or abnormality is detected, they will explain the nature of the condition, its severity, and any potential medical or lifestyle interventions that might be necessary.
- Decision-Making: Depending on the results, you may need to make decisions about the continuation of the pregnancy, additional diagnostic tests, medical interventions, or planning for the care of a child with special needs. Your healthcare provider will provide guidance and support throughout this process.
- Additional Testing or Consultations: Depending on the results and the specific condition detected, your healthcare provider might recommend further testing, such as more comprehensive genetic testing, additional ultrasounds, or consultations with specialists.
- Emotional Support: Receiving genetic testing results, especially if they indicate a genetic disorder, can evoke a range of emotions. Your healthcare provider or a counselor can offer emotional support and resources to help you navigate these feelings.
- Continued Prenatal Care: Regardless of the results, your prenatal care will continue. Regular appointments with your obstetrician or midwife, routine ultrasounds, and other prenatal care measures will remain important to monitor the health and development of the fetus.
- Long-Term Planning: If the results indicate a genetic disorder, you may need to begin planning for the care of a child with special needs. This might involve connecting with support groups, seeking guidance from medical specialists, and making preparations for your family’s future.
Ethical and Social Considerations:
Here are some key ethical and social considerations associated with CVS.
- Reproductive Autonomy: One of the primary ethical considerations is the principle of reproductive autonomy, which emphasizes an individual’s right to make informed decisions about their reproductive choices. This includes the decision to undergo genetic testing and make choices based on the test results.
- Informed Consent: Ensuring that individuals and couples have a clear understanding of the benefits, risks, and implications of CVS is essential. Informed consent allows individuals to make decisions that align with their values and preferences.
- Non-Directive Counseling: Genetic counselors and healthcare providers should provide unbiased information and counseling, presenting all available options without imposing their own values or opinions on individuals or couples.
- Confidentiality and Privacy: Genetic testing involves sensitive and personal information. Maintaining confidentiality and protecting privacy are crucial to respecting individuals’ rights and ensuring trust in the healthcare system.
- Stigmatization and Discrimination: Genetic testing results, especially if they indicate the presence of a genetic disorder, can lead to stigmatization and discrimination. This might impact how individuals and families are perceived by society or within their communities.
- Cultural and Religious Beliefs: Different cultures and religions have varying beliefs about prenatal testing, abortion, and the value of life. Healthcare providers need to be sensitive to cultural and religious perspectives when discussing genetic testing options.
- Selective Abortion: When genetic abnormalities are detected, some individuals might choose to terminate the pregnancy. The ethical implications of selective abortion raise questions about when life begins and the value of life with disabilities.
- Parental Responsibility: The decision to continue a pregnancy despite a detected genetic disorder reflects a commitment to caring for a child with special needs. This decision can lead to a redefinition of parental roles and responsibilities.
- Equitable Access: Ensuring that all individuals, regardless of socioeconomic status or geographic location, have equitable access to genetic testing and counseling is essential for promoting justice and fairness.
- Impact on Family Dynamics: Genetic testing results can influence family dynamics, relationships, and decisions about future pregnancies. The implications of these results can reverberate through the family unit.
FAQs:
What is Chorionic Villus Sampling (CVS)?
CVS is a medical procedure used during pregnancy to obtain a sample of tissue from the placenta, specifically the chorionic villi. This tissue contains genetic material that can be analyzed to assess the genetic health of the fetus.
When is CVS usually performed?
CVS is typically performed between the 10th and 13th weeks of pregnancy. This timing allows for early detection of genetic abnormalities.
What are the reasons for undergoing CVS?
CVS is recommended in cases of advanced maternal age, positive screening tests, previous child with a genetic condition, family history of genetic disorders, parental carriers of genetic disorders, known chromosomal abnormalities in a parent, and other risk factors.
What are the main risks associated with CVS?
The main risks include a small risk of miscarriage (around 0.5% to 1%), procedure-related discomfort, procedure-related complications (such as infection or bleeding), and the emotional impact of receiving test results.
What are the alternatives to CVS?
Alternatives include amniocentesis, non-invasive prenatal testing (NIPT), ultrasound screening, carrier screening, preimplantation genetic testing (PGT), and clinical evaluation and monitoring.
How long does it take to receive CVS test results?
The time it takes to receive results can vary, but your healthcare provider will provide an estimate. Some initial results might be available relatively quickly, while more comprehensive testing might take longer.
What happens after receiving CVS results?
After receiving results, you’ll have a follow-up appointment with your healthcare provider or genetic counselor. They will explain the results, discuss implications, and guide you through any necessary next steps.
What are the ethical considerations of CVS?
Ethical considerations include reproductive autonomy, informed consent, non-directive counseling, confidentiality, cultural and religious beliefs, stigmatization, and selective abortion.
How can I prepare for the decision to undergo CVS?
Gather information about CVS, consult healthcare providers, genetic counselors, and consider your risk factors, values, and preferences. Ensure you have a support system in place.
Is genetic counseling recommended before CVS?
Yes, genetic counseling is often recommended before undergoing CVS. Genetic counselors provide information, answer questions, and help individuals and couples make informed decisions.
Conclusion:
In conclusion, Chorionic Villus Sampling (CVS) stands as a significant diagnostic tool in prenatal care, offering insights into the genetic health of the developing fetus through the collection and analysis of placental tissue. While providing valuable information about potential genetic abnormalities, CVS necessitates careful consideration due to its associated risks and ethical implications. The decision to undergo CVS should be guided by thorough discussions with healthcare professionals and genetic counselors, taking into account individual risk factors, preferences, and the broader emotional, ethical, and societal considerations surrounding prenatal genetic testing.






