An abscess is a localized collection of pus that forms within tissues in the body. Pus is a thick fluid composed of dead white blood cells, tissue debris, and bacteria. Abscesses can develop in various parts of the body, including the skin, internal organs, and even in the brain. They are often painful and may present with swelling, redness, warmth, and tenderness at the affected site.
Definition of an Abscess.
An abscess is a localized collection of pus that forms within the body, typically in response to an infection or foreign material. Pus is a thick, yellowish or greenish fluid composed of dead white blood cells, tissue debris, and bacteria. Abscesses can occur in various parts of the body, including the skin, internal organs, and other tissues.
The formation of an abscess is the body’s natural response to infection. When the immune system detects an invading pathogen, such as bacteria, it sends white blood cells to the site to combat the infection. In the process, these white blood cells, along with damaged tissue and bacteria, accumulate and form a pocket of pus. This collection of pus can cause swelling, redness, warmth, tenderness, and often pain in the affected area.
Causes of Abscesses:
Here are the primary causes of abscesses.
- Bacterial Infections: Bacterial infections are the most common cause of abscesses. When bacteria invade the body through a break in the skin or through internal sources, they can trigger the immune response, leading to the formation of an abscess. Common bacterial causes include Staphylococcus and Streptococcus species.
- Foreign Bodies: Sometimes, foreign materials, such as splinters, thorns, or even piercing jewelry, can introduce bacteria into the body. These foreign bodies can become lodged in tissues, causing inflammation and infection, which may result in an abscess.
- Blocked Glands: Certain types of abscesses, like a sebaceous cyst or a Bartholin’s gland cyst, can form when a gland or duct in the body becomes blocked, allowing fluids to accumulate and create a pocket of infection.
- Infected Wounds: Open wounds, whether from injuries, surgical procedures, or medical devices, are susceptible to bacterial contamination. If bacteria enter a wound, it can lead to wound infections and the formation of an abscess.
- Dental Infections: Dental abscesses can occur when there is an infection in a tooth, the gums, or the surrounding jawbone. These abscesses are often painful and may require dental treatment.
- Systemic Infections: Certain systemic infections can lead to the development of internal abscesses, such as liver abscesses or lung abscesses, when the infection spreads to other parts of the body.
- Inflammatory Conditions: Some inflammatory conditions, like Crohn’s disease, can lead to abscess formation in the gastrointestinal tract.
- Infected Hair Follicles: Folliculitis is an infection of hair follicles that can lead to the formation of small abscesses. This is a common condition in which hair follicles become inflamed and infected.
Signs and Symptoms:
Here are typical signs and symptoms of an abscess.
- Localized Swelling: The affected area will often appear swollen and may feel firm to the touch. The swelling can vary in size, from small and barely noticeable to large and prominent.
- Redness and Warmth: The skin over the abscess is usually red and warm to the touch due to the inflammatory response. This is caused by increased blood flow to the area.
- Tenderness and Pain: Abscesses are often painful. The pain can range from mild discomfort to severe and throbbing, especially when pressure is applied to the area.
- Pus Formation: As the abscess matures, it may become visibly filled with pus, which is a thick, yellowish or greenish fluid. If the abscess is close to the skin surface, you may notice a visible “head” or pustule.
- Fever: In some cases, especially if the infection is more severe or has spread, an individual may develop a fever. This is a systemic response to the infection.
- General Malaise: An abscess can make a person feel generally unwell, with symptoms such as fatigue, loss of appetite, and sometimes chills.
- Change in Skin Sensation: Some abscesses can cause a change in skin sensation, like itching, tingling, or numbness in the affected area.
- Drainage: When an abscess begins to spontaneously drain, you may notice the release of pus and a reduction in pain and swelling. The drainage may be white, yellow, or green, and it can have an unpleasant odor.
- Symptoms Related to the Site of the Abscess: The signs and symptoms can vary depending on where the abscess is located. For example, dental abscesses may cause toothache, while lung abscesses may lead to coughing and difficulty breathing.
Diagnosis:
- Clinical Examination: A healthcare provider will begin by examining the affected area. They will assess the patient’s medical history, ask about symptoms, and inspect the area for signs of an abscess, such as localized swelling, redness, warmth, tenderness, and visible pus. They may also inquire about recent injuries, surgeries, or other potential sources of infection.
- Physical Examination: The healthcare provider will perform a physical examination to assess the overall health of the patient. They may check for signs of systemic infection, such as fever, chills, or increased heart rate.
Imaging Studies:
- Ultrasound: An ultrasound can provide real-time imaging of the abscess, helping to determine its size and location. It is often used for superficial or easily accessible abscesses.
- CT Scan (Computed Tomography): A CT scan can provide detailed images of deeper or internal abscesses. It is particularly useful for assessing the extent of internal abscesses, like liver or lung abscesses.
- MRI (Magnetic Resonance Imaging): An MRI may be used in some cases to visualize the abscess, especially if it involves soft tissues or the brain.
Laboratory Tests:
- Blood Tests: Blood tests can help identify signs of infection, such as an elevated white blood cell count. They can also indicate the presence of systemic infection.
- Culture and Sensitivity Tests: If pus or fluid is aspirated from the abscess during drainage, it can be sent to a laboratory for culture and sensitivity testing. This helps identify the specific bacteria causing the infection and determine the most effective antibiotics for treatment.
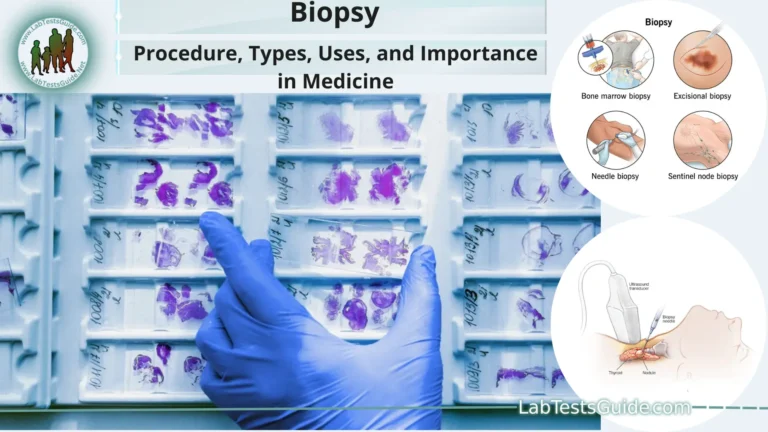
- Biopsy (if necessary): In some cases, a tissue sample (biopsy) may be taken from the abscess for further examination and to rule out underlying conditions.
Prevention:
Here are some strategies to help prevent abscess formation.
- Hand Hygiene: Proper handwashing with soap and water is one of the most effective ways to prevent the spread of bacteria. Wash your hands regularly, especially before handling food, after using the bathroom, and after contact with potential sources of infection.
Wound Care:
- Clean Wounds: If you have a cut, scrape, or puncture wound, clean it promptly with soap and water to reduce the risk of infection.
- Cover Wounds: Keep wounds covered with a clean bandage or dressing to protect them from dirt and bacteria.
- Change Dressings: Change dressings on wounds regularly and keep them clean and dry.
- Maintain Good Dental Hygiene: Dental infections, including abscesses, can be prevented by practicing good oral hygiene. Brush and floss your teeth regularly, and visit your dentist for check-ups and cleanings.
- Proper Piercing and Tattoo Care: If you have piercings or tattoos, follow proper aftercare instructions to reduce the risk of infection. Keep the area clean and avoid touching it with dirty hands.
- Avoid Sharing Personal Items: Do not share personal items such as razors, towels, or personal hygiene items that can potentially carry bacteria.
- Skin Care: Maintain healthy skin by keeping it clean and moisturized. Avoid picking at or squeezing pimples or other skin blemishes, as this can introduce bacteria and lead to skin abscesses.
- Manage Chronic Conditions: If you have underlying medical conditions that increase your risk of abscesses (e.g., diabetes or immunosuppressive conditions), work with your healthcare provider to manage these conditions effectively.
- Safe Injection Practices: If you require injections or medical procedures involving needles, make sure they are administered in a healthcare setting using sterile equipment.
- Proper Hygiene in Healthcare Settings: If you work in a healthcare setting, follow proper infection control practices, including hand hygiene, wearing personal protective equipment, and maintaining a clean environment.
- Avoid Intravenous Drug Use: If you use intravenous drugs, seek help to quit, as this is a significant risk factor for developing skin and soft tissue abscesses.
- Seek Prompt Treatment: If you notice any signs of infection or abscess formation, seek prompt medical attention. Early treatment can help prevent the progression of the infection.
- Vaccinations: Some vaccinations, such as the tetanus vaccine, can help prevent abscesses resulting from certain injuries. Make sure your vaccinations are up-to-date.
Treatment:
Here are the primary methods used in the treatment of abscesses.
Incision and Drainage (I&D):
- Local Anesthesia: Before the procedure, the area around the abscess is usually numbed with a local anesthetic to minimize pain and discomfort.
- Incision: A healthcare provider makes a small incision (cut) into the abscess to create an opening for the pus to drain out. This relieves pressure and reduces pain and swelling.
- Drainage: The pus and infected material are gently expressed or drained from the abscess, often with the help of sterile gauze or a syringe. The wound is cleaned, and any debris or necrotic tissue is removed.
- Dressing: After drainage, the wound may be left open or packed with gauze to continue draining. In some cases, it may be sutured or closed partially.
- Needle Aspiration: For smaller, less severe abscesses, a needle and syringe can be used to withdraw pus from the abscess without making a surgical incision. This procedure is often done under local anesthesia and is less invasive than I&D.
- Antibiotics: In some cases, antibiotics may be prescribed to treat the underlying infection or to prevent the spread of infection to other parts of the body. The choice of antibiotics depends on the type of bacteria causing the infection and their sensitivity to specific antibiotics. Antibiotics are typically used in addition to drainage for internal or systemic abscesses.
- Surgical Intervention: In cases where abscesses are particularly large, deep, or complex, or if there is an associated complication, surgical procedures may be necessary. This could involve the removal of the source of infection, repair of damaged tissue, or other interventions to manage the condition effectively.
- Pain Management: Pain relief measures, such as over-the-counter pain medications or prescription painkillers, may be prescribed to manage discomfort during the recovery period.
- Follow-up Care: After treatment, it’s important to follow up with your healthcare provider to monitor the healing process. They will ensure that the abscess has fully resolved, and the wound is healing correctly.
Complications:
Some of the potential complications associated with abscesses include.
- Cellulitis: Cellulitis is a bacterial skin infection that can develop when the infection from an abscess spreads to the surrounding skin. It can cause redness, swelling, and pain in the affected area and may require additional treatment.
- Systemic Infection: If the bacteria from an abscess enter the bloodstream, it can lead to a systemic infection called sepsis. Sepsis is a life-threatening condition that can cause fever, rapid heartbeat, low blood pressure, confusion, and multiple organ failure.
- Fistula Formation: In some cases, an abscess may create a tunnel-like connection (fistula) between two organs or between an organ and the skin. Fistulas can lead to ongoing drainage, recurrent infections, and may require surgical intervention to repair.
- Localized Tissue Damage: The pressure and inflammation from an abscess can cause damage to nearby tissues, leading to scarring, impaired function, or disfigurement.
- Spread to Other Organs: Internal abscesses can lead to infection and damage to vital organs. For example, a liver abscess may spread to the bloodstream and affect multiple organs.
- Recurrence: Even after successful treatment, some abscesses have a tendency to recur, especially if the underlying cause, such as chronic skin conditions or an obstructed gland, is not addressed.
- Nerve Damage: Abscesses near nerves can potentially damage these nerves, leading to numbness, weakness, or altered sensation in the affected area.
- Respiratory Complications: Lung abscesses can cause coughing, shortness of breath, and chest pain, and if not treated, they can lead to severe respiratory issues.
- Brain Abscess Complications: Brain abscesses can be particularly dangerous and may lead to neurological deficits, seizures, or life-threatening intracranial pressure if left untreated.
- Septic Arthritis: Abscesses near a joint can lead to septic arthritis, which can cause joint pain, swelling, and loss of joint function.
- Complications Related to Surgical Interventions: Surgical drainage or removal of an abscess may carry risks, including wound infection, bleeding, or scarring.
When to Seek Medical Attention:
Here are some key situations in which you should seek medical care for an abscess.
- Increasing Pain and Swelling: If the abscess is causing severe or increasing pain and swelling, it’s an indication that it may be getting worse. This is especially important if the pain is interfering with your daily activities or sleep.
- Fever: If you develop a fever along with the abscess, it can be a sign of a spreading infection. A fever is a systemic response to infection and should not be ignored.
- Redness and Warmth: If the skin around the abscess becomes increasingly red and warm, it suggests that the infection is spreading beyond the localized area.
- Enlarging Abscess: If the abscess continues to grow in size, it may indicate that it’s not spontaneously draining or responding to home care, and professional intervention is needed.
- Multiple Abscesses: If you have multiple abscesses in different areas of your body or if you’ve had recurring abscesses, it’s essential to see a healthcare provider to determine if there’s an underlying condition contributing to their formation.
- Pus Drainage: If the abscess begins to spontaneously drain or if you notice an increase in pus drainage, it may be a sign that the abscess is ready for medical attention.
- Location: Abscesses in certain areas, such as the face, hands, genitals, or near major joints, may require prompt medical care due to the potential for complications.
- Systemic Symptoms: If you experience symptoms like chills, confusion, weakness, or nausea in addition to the abscess, it may indicate a systemic infection or sepsis, which requires immediate medical attention.
- Underlying Health Conditions: If you have underlying health conditions that weaken your immune system, such as diabetes or HIV, or if you’re taking immunosuppressive medications, it’s essential to seek medical care promptly.
- Persistent Symptoms: If the abscess does not improve or resolve after several days of home care or if it recurs frequently, medical evaluation is necessary to address any underlying issues.
- Children and the Elderly: Abscesses in young children or the elderly should be evaluated by a healthcare provider due to their vulnerability to complications.
FAQs:
What is an abscess?
An abscess is a localized collection of pus that forms within the body, often in response to an infection, injury, or foreign material.
What causes abscesses?
Abscesses are typically caused by bacterial infections, but they can also result from foreign bodies, blocked glands, or other factors.
What are the common signs and symptoms of an abscess?
Common symptoms include localized swelling, redness, warmth, tenderness, pain, and the formation of pus. Systemic symptoms can include fever and malaise.
How are abscesses diagnosed?
Diagnosis typically involves clinical examination, imaging studies (e.g., ultrasound, CT scans), laboratory tests (e.g., blood tests, culture and sensitivity), and sometimes a biopsy.
What is the treatment for an abscess?
Treatment often involves incision and drainage (I&D) or needle aspiration to remove pus, along with antibiotics to treat the underlying infection. Surgical intervention may be necessary in some cases.
Can I treat an abscess at home?
Small, uncomplicated abscesses may be managed at home with warm compresses and good wound care. However, it’s essential to seek medical attention for proper evaluation, especially for larger or severe abscesses.
Are there complications associated with abscesses?
Yes, abscesses can lead to complications such as cellulitis, systemic infection (sepsis), fistula formation, tissue damage, and the spread of infection to other organs.
How can I prevent abscesses?
Preventing abscesses involves good hygiene practices, wound care, managing underlying conditions, and seeking prompt medical attention for any injuries or infections.
When should I seek medical attention for an abscess?
You should seek medical attention if the abscess is causing severe pain, has systemic symptoms like fever, is enlarging, or is in a critical location (e.g., face or genitals). Recurring or persistent abscesses also require medical evaluation.
What is the difference between an abscess and a boil?
A boil is a specific type of abscess that forms within a hair follicle or oil gland. While the terms are often used interchangeably, boils are a subset of abscesses.
Can abscesses be prevented in children?
Good hygiene practices and prompt care for cuts and scrapes can help prevent abscesses in children. Parents should also be vigilant about any recurring or unusual skin conditions.
Can abscesses recur?
Yes, abscesses can recur, especially if the underlying cause, such as a chronic skin condition or blocked gland, is not addressed. Recurrent abscesses should be evaluated by a healthcare provider.
Conclusion:
In conclusion, abscesses are localized collections of pus that develop in response to infections, injuries, or other factors and can lead to a range of symptoms and potential complications. Timely medical evaluation, appropriate treatment, and good wound care are essential to manage abscesses effectively and prevent further health issues. While smaller abscesses may be managed with home care, larger or severe abscesses, those in critical locations, or those with systemic symptoms warrant immediate medical attention to ensure a safe and successful resolution of the condition and to prevent complications like cellulitis, sepsis, or tissue damage.