Blood Urea Nitrogen Test Purpose, procedure, Result Interpretation and Your Test Result Meaning
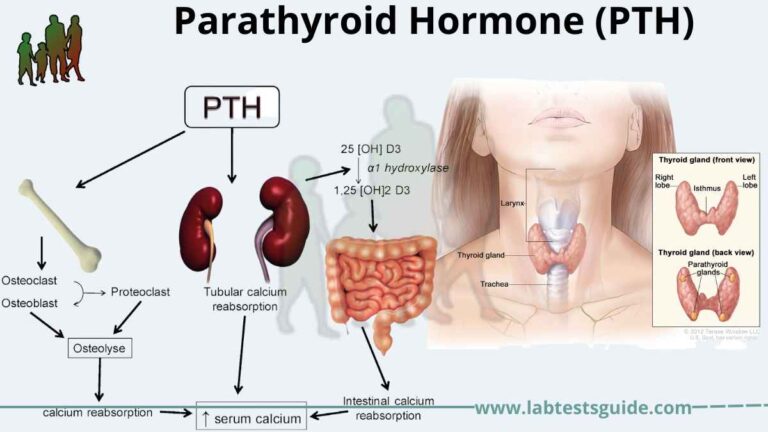
Blood urea nitrogen (BUN) is a laboratory test that measures the amount of urea nitrogen in the bloodstream. Urea is a waste product produced in the liver when the body breaks down proteins. It is then filtered out of the blood by the kidneys and excreted in the urine. The BUN test is commonly performed to assess kidney function and evaluate the body’s nitrogen balance.
Understand Your Test Results:
Understand your Blood Urea Nitrogen Test Results
AI-powered Lab Test Results Meaning tool 🤖
| Also Known as | BUN, Urea Nitrogen, Blood Urea Notrogen, Serum BUN, Urea Nitrogen Test |
| Test Purpose | BUN is a measurement of the Nitrogen in the bloodstream. |
| Test Preparations | No Special Preparation Required. |
| Test Components | BUN, Blood Urea |
| Specimen | 2 ML (0.5 ML Min.) Serum From 1 SST. Ship Refrigerated Or Frozen. |
| Stability Room | 2 Hours |
| Stability Refrigerated | 1 Week |
| Stability Frozen | 2 Weeks |
| Method | Routein Chemistry |
| Download Report | Download Report |
BUN levels tend to increase when the kidneys or liver are damaged. Having too much urea nitrogen in the blood can be a sign of kidney or liver problems.
Panel Tests: Urea, Blood Urea Nitrogen, Creatinine, Calcium, Phosphorus, Albumin, Magnesium, Total Protein, Electrolytes
Why Get Tested:
- To assess the renal function.
- As a routine test in the patient with dialysis.
- To assess liver function.
- This may be part of the routine test.
- In patients:
- Has nonspecific symptoms.
- During the hospital stay.
- Prior to some drug therapy.
- Acutely ill patient admitted in an emergency.
When to get Tested:
- As part of a routine comprehensive or basic metabolic panel (CMP or BMP) during a health exam.
- When you have signs and symptoms that may be due to kidney disease or you have a condition that may cause or be worsened by kidney dysfunction.
- At regular intervals when you are being treated for kidney disease or damage.
Sample Required:
- This is done on the serum of the patient.
- No special preparation is needed.
Precautions for Sample:
- If there is Fluoride that will inhibit Urease reaction.
- Avoid hemolysis.
- Protein intake will affect BUN. Low protein diet will give low BUN.
- High protein diet or nasogastric tubing will increase BUN.
- Keep in mind muscle mass which is more in males than females and children.
- Overhydrated patient will dilute the BUN and gives a lower value.
- The dehydrated patient will concentrate BUN and gives high value.
- GI bleeding can cause an increase in BUN level.
- Advanced pregnancy may increase the BUN level.
- Drugs increasing the BUN level are cephalosporin, indomethacin, gentamicin, polymyxin B, rifampicin, bacitracin, neomycin, tetracycline, thiazide diuretics, and aspirin.
- There are drugs which decrease the BUN level are streptomycin and chloramphenicol.
Normal Ranges:
- Urea = 20 to 40 mg/dl
- Blood urea nitrogen (BUN) = 10 to 20 mg /dl
Increased Urea (BUN) Azotemia seen in:
A. Impaired renal function:
Prerenal causes:
- congestive heart failure and Myocardial infarction (CHF).
- Salt and water depletion
- Shock
- Stress
- Acute MI
- Hemorrhage into GI tract
- Dehydration.
- excessive protein catabolism.
- Burn.
B. Chronic renal diseases:
Renal causes
- Glomerulonephritis (GN).
- Pyelonephritis (PN).
- Acute tubular necrosis.
- Renal failure.
- Diabetes mellitus with ketoacidosis.
- Anabolic steroids use.
- Nephrotoxic drugs.
C. Urinary tract obstruction:
Postrenal causes
- Ureteral obstruction from stones, tumors, or congenital abnormality.
- Bladder outlet obstruction from prostatic hypertrophy, cancer.
- Bladder / urethral congenital abnormality.
Decreased Urea (BUN) seen in:
- Liver failure.
- Malnutrition, and low protein diet.
- Impaired absorption of Celiac disease.
- Syndrome of inappropriate antidiuretic hormone secretion.
- Pregnancy.
- Overhydration.
- Nephrotic syndrome.
Effect of drugs and other condition on a BUN:
- Some of the drugs may cause a decrease in BUN like Dextrose infusion, Phenothiazine, and Thymol.
- Increased BUN level may be seen in late pregnancy and infancy because of increased use of proteins.
BUN/Creatinine ratio:
- The normal BUN/creatinine ratio is around 10:1.
- BUN/creatinine ratio in the normal range, in the case of raised BUN and creatinine. This will suggest intrarenal disease:
- Glomerulonephritis.
- Tubulointerstitial nephritis.
- When the BUN / Creatinine ratio is raised will suggest:
- Prerenal azotemia.
- Postrenal azotemia.
- These conditions may be seen in hypovolemia or hypotension.
- BUN/creatinine ratio decreased is very rare and this may be seen in:
- Protein deficiency in the diet.
- In severe liver disease.
Understand Your Test Results:
Understand your Blood Urea Nitrogen Test Results
AI-powered Lab Test Results Meaning tool 🤖