Salmonella (S. Typhi & NTS): Microbiology, Lab Diagnosis, Culture & Biochemical Tests
The encyclopedic reference for Clinical Microbiologyclinical microbiology, genomics, Biochemical Profiling, and infectious disease management (Typhoid vs. Non-Typhoidal Salmonellosis). Named after Daniel Elmer Salmon.

Complete Taxonomy & Complex Nomenclature
| Domain | Bacteria |
|---|---|
| Phylum | Pseudomonadota (formerly Proteobacteria) |
| Class | Gammaproteobacteria |
| Order | Enterobacterales |
| Family | Enterobacteriaceae |
| Genus | Salmonella |
| Core Species | S. enterica & S. bongori |
| Key Serovars | Typhi, Typhimurium, Enteritidis |
Understanding Salmonella Nomenclature
The taxonomy of Salmonella is notoriously complex. There are only two official species: S. enterica (human pathogen) and S. bongori (primarily associated with cold-blooded animals; rare human infections). S. enterica is further divided into six subspecies.
- Subspecies I (enterica): Causes 99% of human infections.
- Serovars: Within Subspecies I, there are >2,600 serovars (serotypes) classified by the Kauffmann-White scheme.
- Naming Convention: By convention, the genus is italicized, but the serovar is capitalized and NOT italicized. Example: Salmonella enterica serovar Typhi is simply written as Salmonella Typhi.
Morphology & Antigenic Structure
Salmonella species are Gram-negative, facultatively anaerobic, non-spore-forming bacilli (rods). With the exception of S. Gallinarum and S. Pullorum (avian pathogens), all human clinical isolates are highly motile via peritrichous flagella.
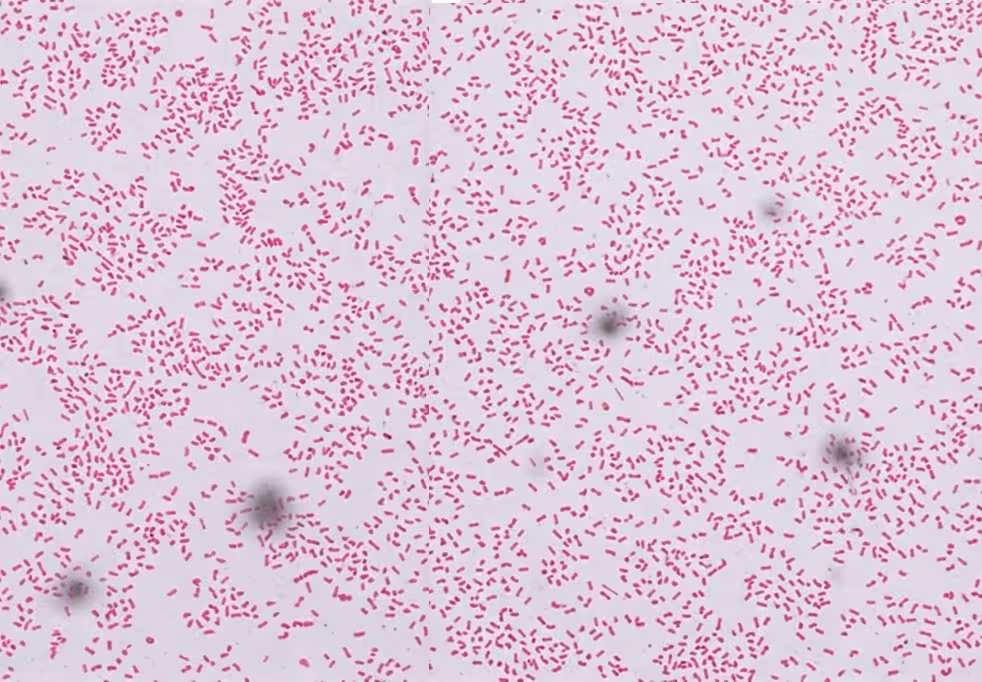
O Antigen (Somatic)
The outermost component of the lipopolysaccharide (LPS) cell wall. It is heat-stable and functions as a potent endotoxin. It determines the serogroup (e.g., Group A, B, C, D) in the Kauffmann-White classification.
H Antigen (Flagellar)
Proteinaceous and heat-labile flagellin. Salmonella is unique because it undergoes Phase Variation—it can alternate between expressing two different flagellar antigen phases (Phase 1 and Phase 2) to evade the host immune system.
Vi Antigen (Capsular)
Stands for “Virulence” antigen. It is a highly specialized capsular polysaccharide found almost exclusively on Salmonella Typhi and S. Paratyphi C. It blocks phagocytosis and masks the O antigen during serotyping.
Comprehensive Culture Media Profiles
MacConkey (MAC) Agar
Result: Colorless, transparent colonies.
Mech: Salmonella is a Non-Lactose Fermenter (NLF). It uses peptones, which increases pH, leaving the neutral red indicator colorless.
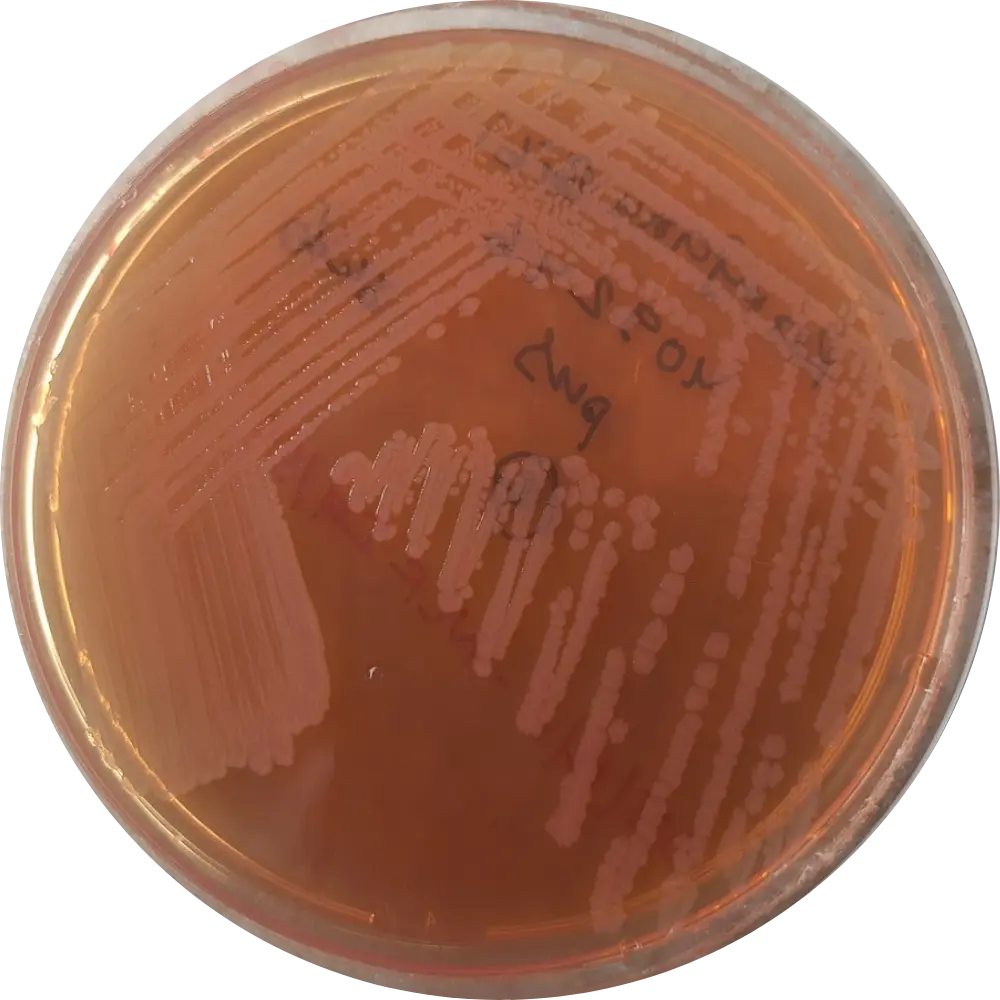
Xylose Lysine Deoxycholate (XLD) Agar
Result: Red colonies with Black Centers.
Mech: Initially ferments xylose (yellow), then lysine decarboxylation restores alkaline pH (red), turning media alkaline (Red). Thiosulfate reduction produces H2S gas (Black center).
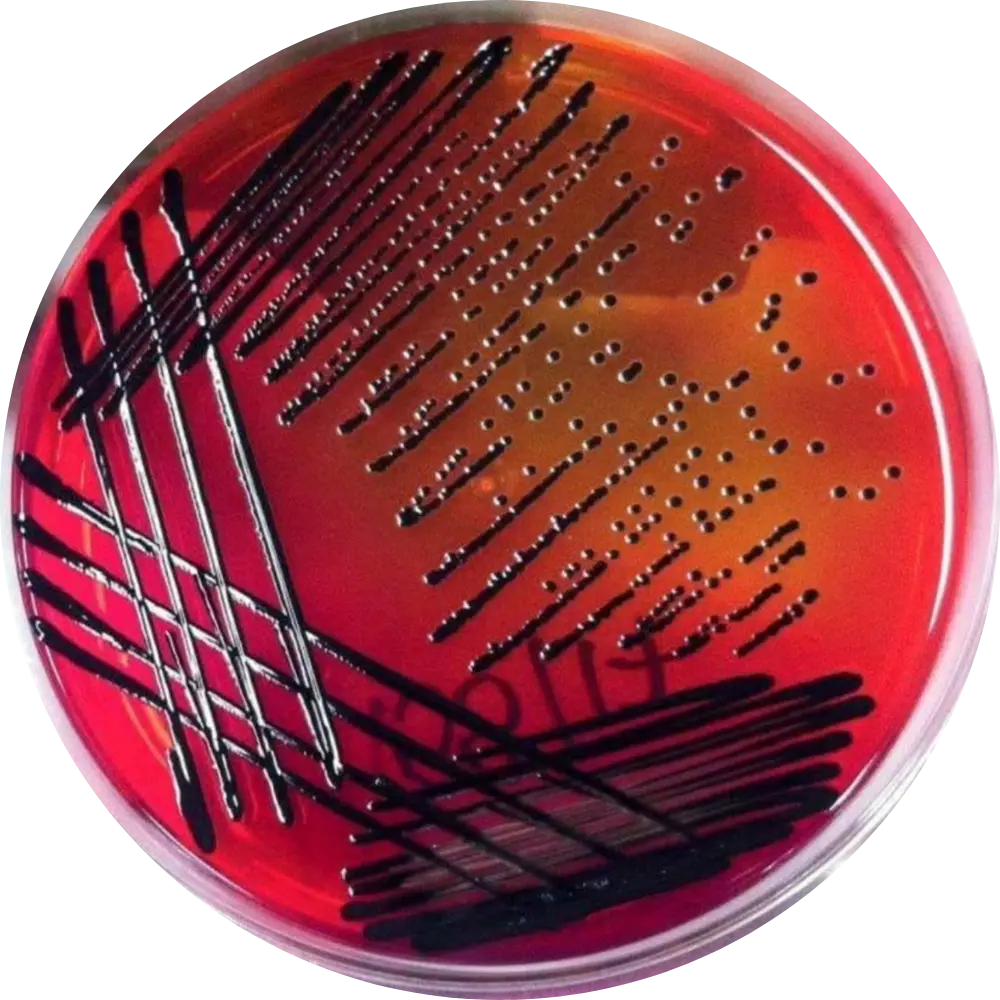
Salmonella-Shigella (SS) Agar
Result: Colorless colonies with black centers.
Mech: Highly selective. Bile salts inhibit Gram-positives. Lactose negative (colorless) and H2S positive (black center).
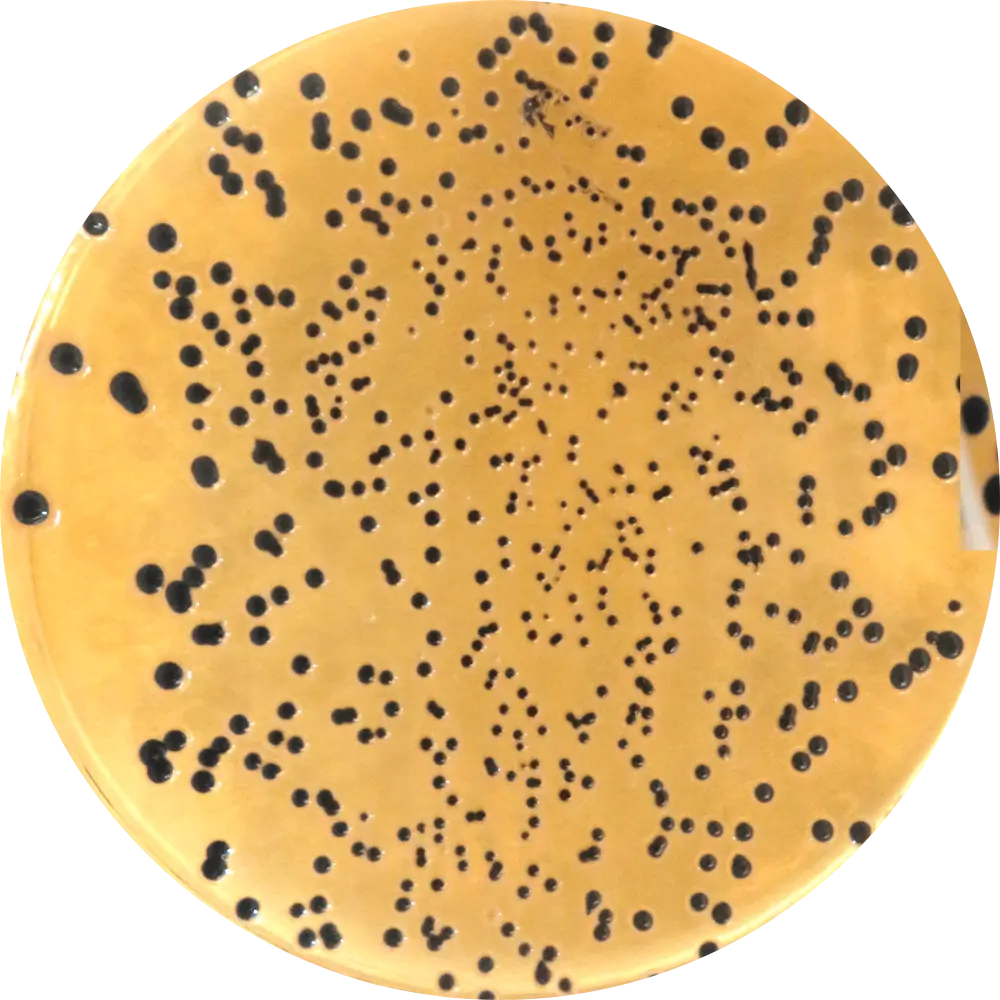
Bismuth Sulfite Agar (BSA)
Result: Black colonies with a Metallic Sheen.
Use: Highly specific for isolating S. Typhi. Bismuth sulfite severely inhibits most other flora.
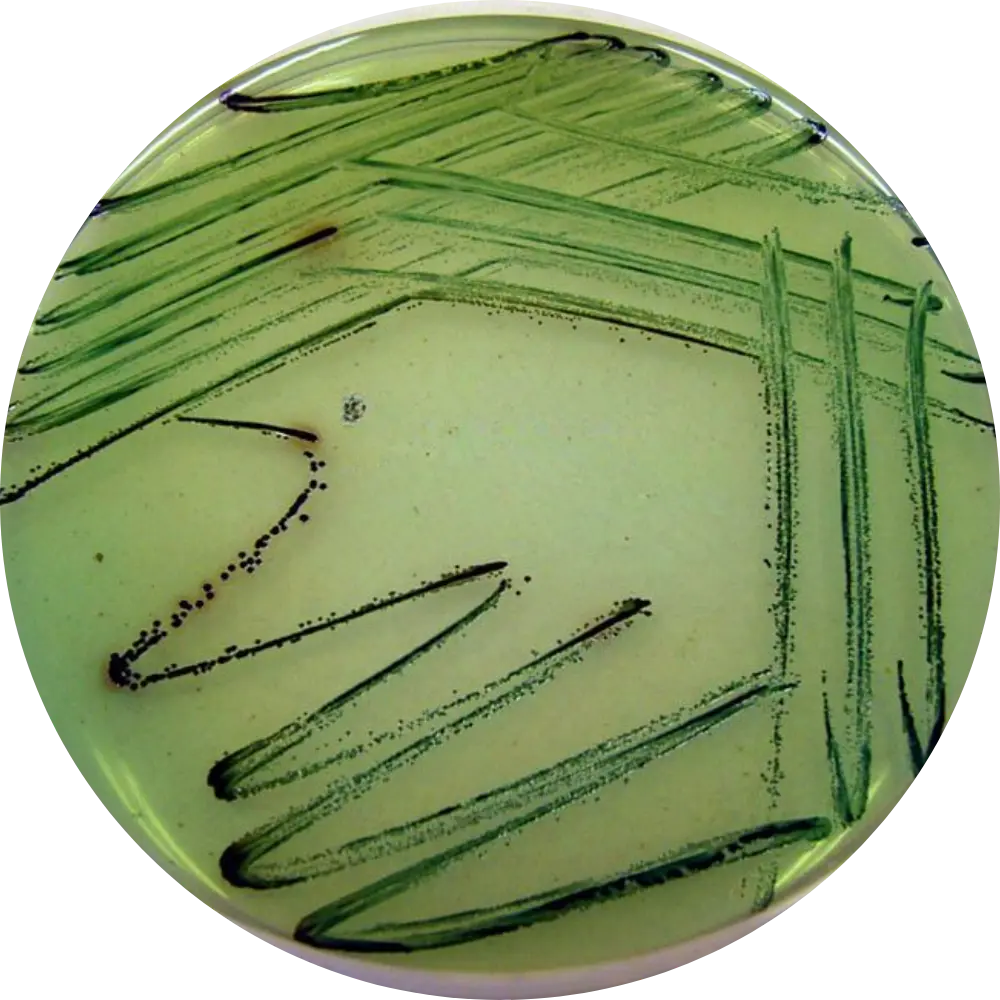
Hektoen Enteric (HE) Agar
Result: Blue-green colonies with black centers.
Mech: NLF (remains blue-green) and H2S producer.
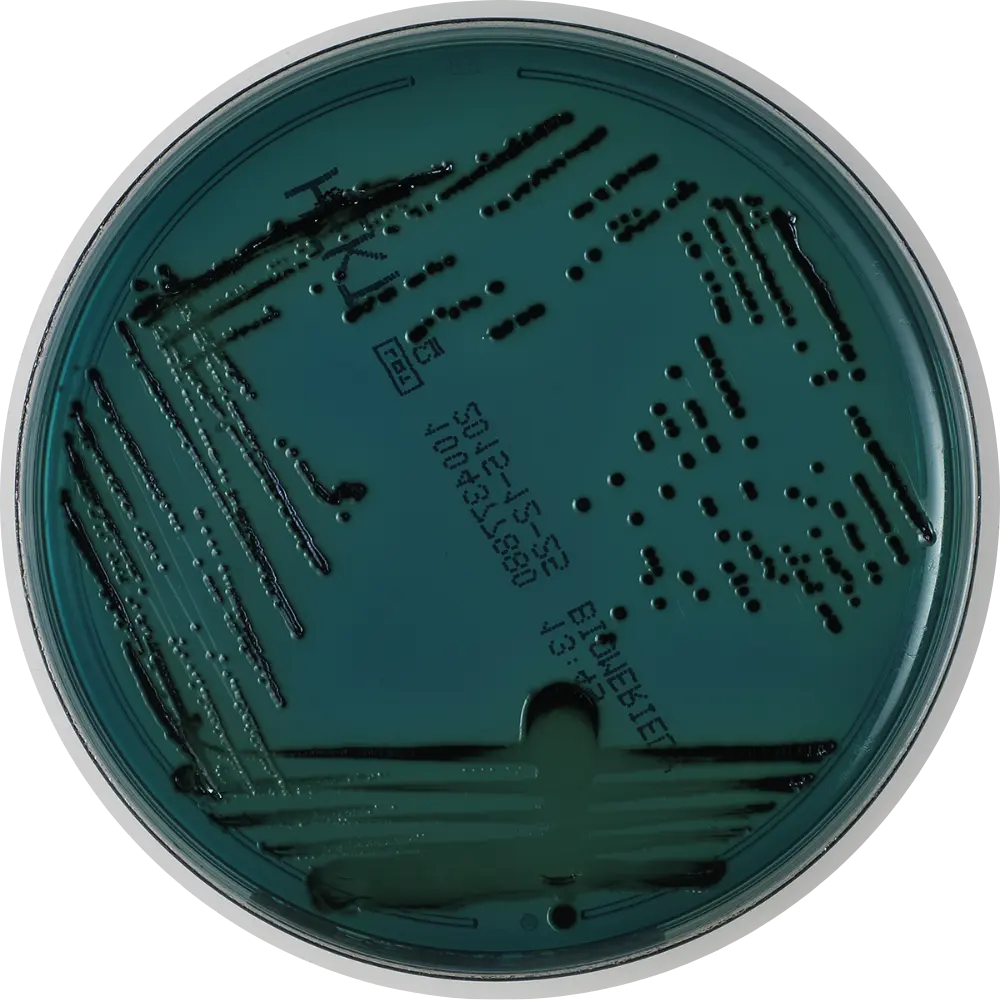
Deoxycholate Citrate Agar (DCA)
Result: Pale, colorless colonies.
Use: Selective for enteric pathogens. NLF appearance.

Colony Morphology (Quick Identification Table)
| Culture Media | Colony Appearance | Key Feature | Interpretation |
|---|---|---|---|
| MacConkey (MAC) | Colorless / Transparent | Non-Lactose Fermenter | No lactose fermentation → no acid → no color change |
| XLD Agar | Red colonies with black centers | H₂S Production | Initial xylose fermentation → lysine decarboxylation → red color + H₂S |
| Salmonella-Shigella (SS) | Colorless with black centers | H₂S Positive | Lactose negative + hydrogen sulfide production |
| Hektoen Enteric (HE) | Blue-green with black centers | H₂S Positive | Non-fermenter (blue-green) + H₂S production |
| Bismuth Sulfite Agar (BSA) | Black colonies with metallic sheen | S. Typhi selective | Strong H₂S production; highly selective for S. Typhi |
| Deoxycholate Citrate Agar (DCA) | Pale / Colorless colonies | Non-Lactose Fermenter | No lactose fermentation; selective for enteric pathogens |
Biochemical Diagnostics: Typhi vs. Non-Typhoidal
A crucial task in the clinical laboratory is distinguishing the highly dangerous S. Typhi from common food-poisoning Non-Typhoidal Salmonella (NTS) like S. Typhimurium or S. Enteritidis.
| Biochemical Test | NTS (e.g., Typhimurium) | Salmonella Typhi | Biochemical Mechanism |
|---|---|---|---|
| Indole | Negative | Negative | Lacks tryptophanase enzyme. |
| Methyl Red (MR) | Positive | Positive | Performs mixed-acid fermentation. |
| Voges Proskauer (VP) | Negative | Negative | Does not produce acetoin. |
| Citrate Utilization | Positive (Blue) | Negative (Green) | Typhi lacks citrate permease, a key differentiating factor. |
| Oxidase | Negative | Negative | Member of Enterobacteriaceae; lacks cytochrome c oxidase enzyme. |
| Catalase | Positive | Positive | Breaks down hydrogen peroxide (H₂O₂) into water and oxygen. |
| TSI Slant / Butt | K / A (Red/Yellow) | K / A (Red/Yellow) | Ferments glucose only; Generally do not ferment lactose (most) or sucrose. |
| TSI Gas Production | Positive (Cracks) | Negative (No Gas) | Typhi is anaerogenic (does not produce gas from glucose). |
| TSI H2S Production | Abundant Blackening | Weak or variable H2S production (often minimal blackening) | Typhi produces very weak H2S compared to NTS. |
| Urease | Negative (Slow) | Negative (Slow) | Key differentiation from rapid urease-positive organisms like Proteus. |
| Motility | Positive | Positive | Highly motile in semisolid media. |
| Lysine Decarboxylase | Positive | Positive | Maintains alkaline environment on XLD agar. |
Mechanisms of Pathogenicity
A. Salmonella Pathogenicity Islands (SPI-1 & SPI-2)
- SPI-1 (Invasion): Encodes a Type III Secretion System (T3SS) that injects effector proteins directly into intestinal M-cells and enterocytes. This causes massive actin cytoskeletal rearrangement, forcing the host cell to engulf the bacteria via membrane ruffling.
- SPI-2 (Survival): Encodes a second T3SS crucial for systemic infection. Once engulfed by macrophages, SPI-2 proteins prevent the fusion of the phagosome with the lysosome. This allows Salmonella to multiply safely inside the Salmonella-Containing Vacuole (SCV) and disseminate throughout the body via the reticuloendothelial system.
B. Endotoxin & Vi Capsular Antigen
- Lipid A Endotoxin: Triggers intense inflammatory responses in the gut (gastroenteritis) and can lead to septic shock in systemic infections.
- Vi Capsular Antigen (Typhi only): Specifically inhibits complement activation and masks the pathogen from neutrophil phagocytosis, allowing S. Typhi to establish severe, long-term systemic infections.
Clinical Pathogenesis & Symptomatology
1. Non-Typhoidal Salmonellosis (NTS)
Causative Agents: S. Typhimurium, S. Enteritidis.
Transmission: Zoonotic foodborne illness. Associated with raw/undercooked poultry, raw eggs, raw milk, and handling reptiles (turtles/iguanas).
Incubation: Rapid onset (6 to 72 hours).
Pathogenesis: Bacteria invade the mucosa of the small/large intestine, causing a massive local inflammatory response (neutrophil infiltration).
Symptoms: Nausea, vomiting, severe abdominal cramps, fever, and non-bloody diarrhea (can occasionally be bloody). Usually self-limiting within 4-7 days.
Complications: Reactive arthritis (Reiter’s syndrome) months after infection.
2. Typhoid (Enteric) Fever
Causative Agents: S. Typhi and S. Paratyphi A, B, C.
Transmission: Strictly human-to-human via the fecal-oral route (contaminated food/water). Endemic in developing nations.
Incubation: 1 to 3 weeks.
Pathogenesis: Penetrates gut mucosa, survives inside macrophages, and disseminates systemically via the lymphatics into the liver, spleen, and bone marrow.
Symptoms: Stepwise escalating high fever, relative bradycardia, abdominal pain, hepatosplenomegaly, and transient faint pink macules on the trunk known as “Rose Spots.”
Chronic Carriage: 1-5% of patients become asymptomatic chronic carriers, harboring the bacteria in their Gallbladder (e.g., “Typhoid Mary”).
Laboratory Diagnosis Workflow
Step 1: Specimen Collection by Disease Stage (Typhoid)
For Typhoid Fever, the location of the bacteria shifts depending on the week of infection:
- Week 1: Blood cultures are positive (bacteremia phase).
- Week 2 & 3: Stool cultures and Urine cultures become positive as the bacteria shed from the gallbladder.
- Bone Marrow Aspirate: The most sensitive diagnostic test at any stage, even after antibiotic initiation.
Step 2: Serotyping & The Widal Test
- Kauffmann-White Serotyping: Isolates are subjected to polyvalent and monovalent antisera via slide agglutination to determine the exact O, H, and Vi antigens. Note: If the Vi capsule is thick, it blocks O antigen agglutination. The isolate must be boiled for 15 minutes to destroy the Vi antigen and unmask the O antigen.
- Widal Test: A historical serological test detecting host antibodies against O and H antigens. A four-fold rise in titer indicates active infection. It is highly cross-reactive and largely replaced by molecular methods today, but still used in endemic regions.
Step 3: Advanced Molecular Diagnostics
Modern clinical laboratories utilize MALDI-TOF MS for rapid identification from culture plates within minutes. Additionally, multiplex PCR panels (e.g., BioFire GI Panel) detect Salmonella DNA directly from stool samples in 1 hour without the need for enrichment broths.
Treatment & Antimicrobial Resistance (AMR)
Treatment Protocols
- Non-Typhoidal Gastroenteritis: Antibiotics are NOT recommended for healthy individuals. They do not shorten the illness and can actually prolong fecal carriage. Treatment is strictly supportive (oral rehydration).
- Typhoid Fever & Invasive NTS: Antibiotics are mandatory and life-saving. Current primary therapies include Ceftriaxone (3rd-gen cephalosporin) or Azithromycin. Ciprofloxacin is used but faces high resistance rates.
- Chronic Carrier State: Long-term ciprofloxacin therapy or Cholecystectomy (surgical removal of the gallbladder) is required to eradicate the carrier state.
The AMR Crisis: XDR Typhi
Extensively Drug-Resistant (XDR) Salmonella Typhi is a global health emergency, particularly originating from regions like Pakistan.
- MDR Typhi: Resistant to historic first-line drugs: Chloramphenicol, Ampicillin, and Trimethoprim-sulfamethoxazole (TMP-SMX).
- XDR Typhi: Resistant to MDR drugs PLUS Fluoroquinolones and 3rd-Generation Cephalosporins (via ESBL gene blaCTX-M-15). Highly reliant on Azithromycin or Carbapenems as a last resort.
Rapid Review: MLS / ASCP Board Pearls
Critical Differentiator
S. Typhi vs NTS: Typhi is Citrate NEGATIVE, produces trace/crescent H2S, and produces NO GAS from glucose.
Media Appearances
XLD & SS: Colorless/Red with Black Centers (H2S+).
HE: Blue-green with Black Centers.
MAC: Colorless (NLF).
Antigen Masking
The Vi Antigen (capsule) masks the somatic O-antigen. If an isolate won’t agglutinate with O-antisera, BOIL the suspension for 15 mins, cool, and re-test.
Clinical Hallmarks
Typhoid: Rose Spots, relative bradycardia, gallbladder carriage.
NTS Zoonosis: Reptiles (turtles), poultry, eggs.











References:
- Centers for Disease Control and Prevention. Salmonella. Retrieved from https://www.cdc.gov/salmonella/index.html
- World Health Organization. Salmonella. Retrieved from https://www.who.int/news-room/fact-sheets/detail/salmonella-(non-typhoidal)
- Food and Drug Administration. Bad Bug Book: Salmonella. Retrieved from https://www.fda.gov/food/foodborne-pathogens/salmonella-salmonellosis
- Mayo Clinic. Salmonella infection. Retrieved from https://www.mayoclinic.org/diseases-conditions/salmonella/symptoms-causes/syc-20355329
- MedlinePlus. Salmonella infections. Retrieved from https://medlineplus.gov/salmonellainfections.html