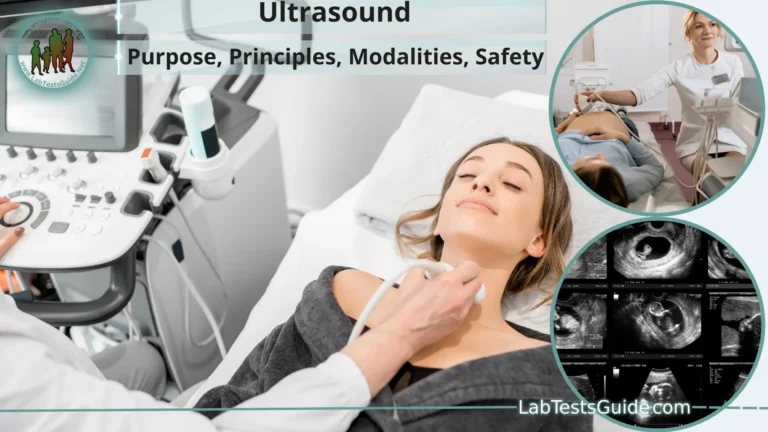
Magnetic Resonance Imaging (MRI) is a medical imaging technique used to visualize the internal structures of the body in detail. It is a non-invasive and non-ionizing imaging modality, which means it does not use radiation like X-rays or CT scans. Instead, MRI relies on the principles of magnetic fields and radio waves to generate detailed images.

- MRI Definition: MRI stands for Magnetic Resonance Imaging, a non-invasive medical imaging technique.
- Imaging Method: It creates detailed images of internal body structures using strong magnets and radio waves.
- Hydrogen Atoms: MRI relies on the behavior of hydrogen atoms in the body’s tissues.
- Alignment: Hydrogen atoms align with the magnetic field during an MRI.
- Pulse Disturbance: Radiofrequency pulses disrupt hydrogen atom alignment.
- Signal Emission: Returning hydrogen atoms emit signals used to create images.
- Machine Components: MRI machines include magnets, RF coils, and gradient coils.
- Magnet Function: Magnets generate the primary magnetic field.
- RF Coils: RF coils transmit and receive radio waves during the scan.
- Gradient Coils: Gradient coils create spatial variations in the magnetic field.
- Types of MRI: Different types include T1-weighted, T2-weighted, and contrast-enhanced MRI.
- Functional MRI (fMRI): Measures brain activity by tracking blood flow changes.
- Diffusion-Weighted MRI (DWI): Assesses tissue microstructure and water diffusion.
- Clinical Use: MRI is vital for diagnosing brain, neurological, musculoskeletal, and cardiovascular conditions.
- Abdominal Imaging: Used to diagnose organ and soft tissue diseases in the abdomen.
- Breast MRI: Helps in breast cancer diagnosis and monitoring.
- Patient Preparation: Fasting may be required for abdominal MRI, and metal objects should be removed.
- Claustrophobia: Options are available for patients who are claustrophobic.
- Stillness Requirement: Patients must remain still during the MRI to avoid artifacts.
- Noise: MRI scans can be noisy, but ear protection is provided.
- Radiation-Free: MRI is non-ionizing and does not use radiation.
- Contrast Agents: Contrast agents are used to enhance visibility of specific tissues.
- Interpretation: Trained radiologists analyze MRI images for diagnosis.
- Safety: MRI is generally safe, but contraindications exist for certain patients.
- Advancements: Ongoing research leads to improvements in MRI technology and capabilities.
Definition of MRI:
MRI stands for Magnetic Resonance Imaging, a medical imaging technique that uses strong magnetic fields and radio waves to create detailed images of the body’s internal structures.
Historical Background:
- Early Magnetic Resonance Research: The principles of magnetic resonance were first described by physicists Felix Bloch and Edward Purcell in the 1940s.
- Nobel Prize: Felix Bloch and Edward Purcell were jointly awarded the Nobel Prize in Physics in 1952 for their contributions to the development of nuclear magnetic resonance (NMR), the precursor to MRI.
- Medical Application Emerges: In the 1970s, researchers began adapting NMR technology for medical imaging.
- First Human MRI Image: The first human MRI image was produced in 1977 by Sir Peter Mansfield and Paul Lauterbur, which earned them the Nobel Prize in Physiology or Medicine in 2003.
- Clinical MRI: The 1980s saw the transition of MRI from a research tool to a clinical imaging technique, initially focusing on brain imaging.
- Widespread Adoption: By the late 1980s and early 1990s, MRI had become a common diagnostic tool in medical practice worldwide.
- Technological Advancements: Ongoing advancements in MRI technology have led to improved image quality, faster scans, and new applications.
- MRI in the 21st Century: MRI continues to evolve, with applications ranging from cancer detection to functional imaging of the brain.
- Safety and Accessibility: Efforts have been made to improve MRI safety and accessibility, including the development of open MRI machines and MRI-compatible medical devices.
- Ongoing Research: Research in MRI is ongoing, with scientists exploring new techniques and applications for this powerful imaging modality.
Purpose of MRI:
The primary purpose of Magnetic Resonance Imaging (MRI) is to visualize the internal structures of the body in detail without the use of ionizing radiation, making it a valuable tool in various medical applications. Here are some key purposes of MRI:
- Medical Diagnosis: MRI is used for diagnosing a wide range of medical conditions and diseases. It provides detailed images of soft tissues, organs, and bones, helping physicians identify abnormalities, tumors, injuries, and infections.
- Brain and Neurological Imaging: MRI is crucial for examining the brain and nervous system. It aids in detecting brain tumors, stroke, multiple sclerosis, and other neurological disorders.
- Musculoskeletal Assessment: MRI is essential for evaluating bones, joints, and soft tissues in the musculoskeletal system. It helps diagnose conditions like ligament tears, joint injuries, and arthritis.
- Cardiovascular Imaging: MRI can assess the structure and function of the heart and blood vessels. It’s used to diagnose heart disease, evaluate blood flow, and assess congenital heart defects.
- Abdominal and Pelvic Imaging: MRI is valuable for diagnosing conditions in the abdomen and pelvis, including liver disease, kidney disorders, and gynecological issues.
- Breast Cancer Detection: Breast MRI is used as a supplementary tool for breast cancer diagnosis, especially in high-risk individuals or when mammograms and ultrasounds provide inconclusive results.
- Functional Imaging: Functional MRI (fMRI) measures brain activity by detecting changes in blood flow. It’s used in neuroscience research and to map brain function in clinical settings.
- Monitoring Disease Progression: MRI is often used to monitor the progression of chronic diseases, such as multiple sclerosis, by visualizing changes in affected tissues over time.
- Preoperative Planning: Surgeons use MRI images to plan complex surgeries, ensuring precision in procedures like tumor removal or joint replacements.
- Research and Development: MRI is a valuable tool in medical research, helping scientists study various aspects of the human body, develop new therapies, and advance medical knowledge.
- Prenatal Imaging: MRI is occasionally used during pregnancy to evaluate fetal anatomy and detect congenital abnormalities.
- Pediatric Imaging: MRI is safe for children and is used to assess various pediatric conditions, including developmental disorders and congenital anomalies.
Applications of MRI:
- Neuroimaging:
- Brain Imaging: MRI is widely used to visualize the brain’s structure and detect abnormalities like tumors, lesions, and vascular issues.
- Functional MRI (fMRI): fMRI measures brain activity by tracking changes in blood flow and is used in neuroscience research and to map brain functions.
- Diffusion Tensor Imaging (DTI): DTI assesses white matter tracts in the brain and is used for studying connectivity and diagnosing conditions like traumatic brain injury.
- Musculoskeletal Imaging:
- Joint Assessment: MRI is crucial for evaluating joint health, diagnosing ligament, tendon, and cartilage injuries, and assessing arthritis.
- Spine Imaging: MRI is used to visualize the spinal cord, discs, and nerve roots, aiding in the diagnosis of conditions like herniated discs and spinal stenosis.
- Muscle and Soft Tissue: It helps diagnose muscle disorders and soft tissue injuries.
- Cardiovascular Imaging:
- Cardiac MRI: This assesses the structure and function of the heart, detecting conditions like myocardial infarction, cardiomyopathy, and congenital heart defects.
- Vascular Imaging: MRI can evaluate blood vessels, including the aorta, carotid arteries, and peripheral arteries, to diagnose vascular diseases.
- Abdominal and Pelvic Imaging:
- Liver and Hepatobiliary Imaging: MRI is used to diagnose liver diseases, evaluate bile ducts, and detect liver tumors.
- Kidney and Urinary Tract Imaging: It helps diagnose kidney disorders and assess urinary tract issues.
- Gynecological and Prostate Imaging: MRI is used to evaluate the female pelvis, including the uterus and ovaries, as well as the prostate gland in men.
- Breast Imaging:
- Breast MRI: This aids in the detection and characterization of breast lesions, often used in breast cancer diagnosis and screening for high-risk individuals.
- Pediatric Imaging:
- MRI is safe for children and is used to diagnose various pediatric conditions, including developmental abnormalities and congenital anomalies.
- Oncology:
- Tumor Characterization: MRI is essential for characterizing tumors, assessing their size, location, and relationship to surrounding tissues.
- Staging: It is used to determine the extent of cancer spread and assess lymph nodes.
- Preoperative Planning:
- Surgeons use MRI images to plan surgeries, ensuring precision in procedures like tumor removal or joint replacements.
- Research and Development:
- MRI is a valuable research tool for studying human anatomy, physiology, and disease processes, leading to advancements in medical knowledge and therapies.
- Prenatal Imaging:
- MRI can be used to evaluate fetal anatomy and detect congenital abnormalities during pregnancy.
Principles of MRI:
- Magnetic Fields: MRI relies on strong magnetic fields, typically generated by superconducting magnets, to create a stable and uniform magnetic environment within the scanner.
- Hydrogen Atoms: The human body is composed mostly of water, which contains hydrogen atoms. MRI primarily detects the behavior of hydrogen nuclei (protons) within these atoms.
- Alignment: In the presence of the magnetic field, hydrogen nuclei align themselves parallel to the field lines.
- Radiofrequency (RF) Pulses: RF pulses, delivered through RF coils, are used to send energy into the body. These pulses can be adjusted to match the resonant frequency of the hydrogen nuclei.
- Resonance: RF pulses disturb the alignment of hydrogen nuclei, causing them to temporarily absorb energy and flip their alignment.
- Relaxation: After the RF pulse is turned off, hydrogen nuclei return to their aligned state, releasing the absorbed energy as radiofrequency signals during a process called relaxation.
- Signal Emission: The emitted RF signals are detected by the RF coils in the MRI machine.
- T1 and T2 Relaxation: There are two main types of relaxation in MRI: T1 (spin-lattice) and T2 (spin-spin). T1 relaxation is the recovery of hydrogen nuclei to their aligned state, while T2 relaxation represents the dephasing of hydrogen nuclei.
- Gradient Coils: Gradient coils create spatial variations in the magnetic field, allowing localization of signals to specific regions in the body.
- Image Reconstruction: A computer processes the detected signals to create detailed cross-sectional images of the body.
- Contrast in MRI: Differences in T1 and T2 relaxation times among tissues create contrast in MRI images, allowing for differentiation of various types of tissues.
- Pulse Sequences: Various pulse sequences, such as spin-echo and gradient-echo, are used to control image contrast and acquire specific types of information.
- Echo Time (TE) and Repetition Time (TR): TE and TR are parameters that can be adjusted in MRI to influence image contrast and acquisition speed.
- Slice Selection: MRI can capture images in multiple planes by selectively exciting slices of tissue along different axes.
- K-Space: K-space is a mathematical representation of the raw data acquired during an MRI scan, which is then transformed into an image through Fourier transformation.
MRI Machine Components:
| Component | Description |
|---|---|
| Magnet | Central component generating a strong and uniform magnetic field. |
| RF (Radiofrequency) Coils | Transmit and receive RF signals for imaging. |
| Gradient Coils | Create spatial variations in the magnetic field for localization. |
| Computer System | Controls the MRI machine, processes data, and generates images. |
| Operator Console | Used by technologists to operate the MRI, set parameters, and monitor scans. |
| Patient Table | The bed or table where the patient lies during the MRI scan. |
| Shielding and RF Cage | Protects against external interference and ensures safety. |
| Cooling System | Maintains the magnet at low temperatures for optimal performance. |
| Power Supply | Provides electrical power to all components of the MRI machine. |
| Display Monitor | Displays images and information for technologists and radiologists. |
| Intercom System | Enables communication between the patient and technologist. |
| Safety Systems | Includes emergency stop buttons and safety protocols to ensure patient safety. |
Patient Preparation:
- Patient Information: The healthcare provider or MRI technologist will gather essential information from the patient, including medical history, current medications, allergies, and any previous surgeries or medical conditions. This information is vital to assess the patient’s suitability for the MRI.
- Contrast Agent Inquiry: If the MRI involves the use of contrast agents (dye), the patient may be asked about allergies or prior adverse reactions to contrast agents. This information helps determine if the patient can safely receive contrast.
- Metal Screening: Patients must inform the technologist and healthcare provider about any metallic objects within their body, such as pacemakers, implants, metal fragments, or medical devices. Some metallic objects can be affected by the MRI’s magnetic field and pose risks to the patient.
- Clothing and Personal Items: Patients will be asked to remove clothing and personal items that contain metal components. They may be provided with a gown to wear during the MRI.
- Jewelry and Accessories: All jewelry, piercings, and accessories, including watches, earrings, necklaces, and belts, should be removed before the scan.
- Makeup and Tattoos: Some cosmetics, particularly those containing metallic pigments, can interfere with the MRI. Patients should avoid wearing makeup or body paint that might contain metallic substances.
- Claustrophobia: Patients who are claustrophobic or anxious about enclosed spaces should inform the healthcare provider. In some cases, sedatives or anxiolytic medications may be prescribed to help the patient relax.
- Fasting Instructions: For specific abdominal MRI exams, patients may be instructed to fast for a period before the scan to improve image quality. The duration of fasting can vary depending on the exam type.
- Fluid Intake: Patients are usually encouraged to drink water before the MRI, unless instructed otherwise. Staying hydrated can help improve image quality and patient comfort.
- Pregnancy: If there is any possibility of pregnancy, patients should inform the healthcare provider or technologist. While MRI is generally considered safe during pregnancy, there are certain precautions and considerations.
- Ear Protection: MRI machines can be noisy, so patients are typically provided with earplugs or headphones to protect their hearing during the scan.
- Patient Education: Patients should be educated about the MRI procedure, including how long it will take and what to expect during the scan. This helps reduce anxiety and ensures cooperation.
- Patient Comfort: Patients should wear comfortable, loose-fitting clothing to enhance their comfort during the MRI.
Safety Considerations:
- Metal Screening:
- All individuals entering the MRI suite must be thoroughly screened for metallic objects or implants, as these can be dangerous in the strong magnetic field of the MRI machine.
- Patients should be questioned about any metallic objects inside their bodies, such as pacemakers, cochlear implants, aneurysm clips, or shrapnel.
- Ferromagnetic Objects:
- The MRI room should be free of ferromagnetic objects, such as oxygen tanks, wheelchairs, and gurneys, which can be strongly attracted to the magnet and pose significant risks.
- Equipment and accessories brought into the MRI suite should be MRI-safe and labeled as such.
- Patient Monitoring:
- Patients should be continuously monitored during the MRI, both visually and through audio communication.
- An emergency call button or intercom system should be readily accessible to patients inside the scanner.
- Contrast Agent Allergies:
- Prior to administering contrast agents, healthcare providers should inquire about allergies or previous adverse reactions to these agents to minimize the risk of allergic reactions.
- Pregnancy:
- Pregnant patients should inform healthcare providers, as MRI during pregnancy may require special precautions and considerations.
- MRI is generally considered safe during pregnancy, especially after the first trimester, but the benefits and risks should be discussed.
- Implant Safety:
- Patients with certain metallic implants may not be eligible for MRI. Healthcare providers should verify implant compatibility and consult with the implant manufacturer or a radiologist if necessary.
- Patient Comfort and Cooperation:
- Patients should be comfortable and informed about the MRI procedure to minimize anxiety and promote cooperation during the scan.
- Sedation and Anesthesia:
- In some cases, sedation or anesthesia may be administered to patients, particularly children or individuals with extreme claustrophobia, to ensure they remain still during the MRI.
- Emergency Preparedness:
- MRI facilities should have well-established emergency procedures in case of accidents or complications during the scan.
- Personnel should be trained in basic life support and first aid.
- Fire Safety:
- Fire extinguishers, which are MRI-safe, should be available in the MRI suite.
- No flammable materials should be present in the MRI environment.
- MRI Technologist Training:
- MRI technologists should receive specialized training in MRI safety, including emergency procedures, patient screening, and equipment operation.
- Noise Protection:
- Patients should be provided with ear protection, such as earplugs or headphones, to reduce noise exposure during the MRI.
- MRI Zones:
- MRI facilities often have designated zones with varying levels of magnetic field strength and safety requirements, and access should be controlled accordingly.
Types of MRI Scans:
Magnetic Resonance Imaging (MRI) offers various types of scans, each designed to provide specific information about the body’s internal structures and functions. Here are some common types of MRI scans:
- T1-Weighted MRI: This scan provides excellent anatomical detail and is often used to visualize the structure of organs and tissues. It is particularly useful for identifying normal vs. abnormal tissue.
- T2-Weighted MRI: T2-weighted images are sensitive to the water content in tissues. They help detect abnormalities like edema, inflammation, and lesions with high water content.
- Contrast-Enhanced MRI: Contrast agents (such as gadolinium) are used to highlight specific tissues or blood vessels. Contrast-enhanced MRI can reveal details not visible in regular scans and is commonly used in vascular and tumor imaging.
- Functional MRI (fMRI): This technique measures changes in blood flow and oxygenation in the brain, providing insight into brain function and activation patterns. fMRI is used in neuroscience research and to map brain functions in clinical settings.
- Diffusion-Weighted MRI (DWI): DWI measures the random motion of water molecules in tissues. It is valuable for detecting abnormalities such as strokes, tumors, and areas of restricted diffusion.
- Perfusion MRI: Perfusion imaging measures blood flow in the brain or other organs. It can help diagnose conditions like stroke and assess tissue viability.
- Magnetic Resonance Angiography (MRA): MRA visualizes blood vessels non-invasively and is used to assess vascular conditions such as aneurysms, stenosis, and arteriovenous malformations.
- Magnetic Resonance Venography (MRV): MRV focuses on the visualization of veins and is used to diagnose venous diseases and conditions, such as deep vein thrombosis (DVT).
- Spectroscopy (MRS): Magnetic Resonance Spectroscopy analyzes the chemical composition of tissues, providing information about metabolites and biomarkers. It is used in research and clinical settings to study brain disorders and cancer.
- Musculoskeletal MRI: Specialized MRI protocols are designed for imaging the musculoskeletal system, including joints, bones, muscles, and tendons. These scans help diagnose sports injuries, arthritis, and orthopedic conditions.
- Breast MRI: Breast MRI is used for breast cancer screening and diagnosis. It can provide detailed information about breast tissue, especially in cases where mammography or ultrasound results are inconclusive.
- Prostate MRI: Prostate MRI is employed to detect and characterize prostate cancer, guide biopsies, and determine the extent of cancer within the prostate gland.
- Pelvic MRI: Pelvic MRI helps diagnose conditions in the pelvic area, including gynecological disorders, prostate issues, and rectal cancer.
- Abdominal MRI: Abdominal MRI is used to evaluate the organs and structures in the abdomen, including the liver, kidneys, spleen, and gastrointestinal tract.
Contrast Agents in MRI:
- Types of Contrast Agents:
- Gadolinium-Based Contrast Agents (GBCAs): These are the most commonly used contrast agents in MRI. Gadolinium chelates are injected intravenously and are typically safe for most patients.
- Superparamagnetic Iron Oxide Nanoparticles (SPIOs): SPIOs are used to enhance liver and spleen imaging and are also used for lymph node imaging.
- Ultrasmall Superparamagnetic Iron Oxide (USPIO): USPIOs are used primarily for imaging lymph nodes and detecting metastases.
- Manganese-Based Contrast Agents: These are used in experimental research and specialized applications.
- Clinical Applications:
- Brain Imaging: GBCAs help visualize brain tumors, lesions, and areas of inflammation, often distinguishing between normal and abnormal tissue.
- Cardiovascular Imaging: GBCAs assist in assessing cardiac function and visualizing blood vessels in magnetic resonance angiography (MRA).
- Abdominal Imaging: GBCAs can highlight liver and spleen lesions, aid in the detection of liver tumors, and improve the characterization of focal liver lesions.
- Musculoskeletal Imaging: Contrast agents can assist in the evaluation of soft tissue lesions, joint abnormalities, and musculoskeletal tumors.
- Breast Imaging: GBCAs are used for breast MRI to evaluate and characterize breast lesions, particularly in cases of equivocal mammography or ultrasound results.
- Tumor Detection: Contrast-enhanced MRI is valuable for detecting and characterizing tumors in various organs and tissues.
- Administration:
- Contrast agents are typically administered intravenously, although some specialized applications involve direct injection into specific body cavities or structures.
- The choice of contrast agent and the timing of administration are tailored to the specific clinical scenario and the type of information required.
- Safety Considerations:
- Gadolinium-based contrast agents are generally considered safe, but there have been concerns about gadolinium retention in the body, particularly in patients with impaired kidney function. Healthcare providers consider the risks and benefits when using these agents.
- Nephrogenic systemic fibrosis (NSF) is a rare but serious condition associated with the use of GBCAs in patients with severe kidney disease.
- Contrast Allergy:
- Some patients may be allergic to contrast agents, particularly GBCAs. Allergic reactions can range from mild to severe. Prior to administration, patients are screened for allergies and a medical history of prior contrast reactions.
- Contrast Agents in Research:
- Researchers continue to develop new types of contrast agents for specialized applications, including molecular imaging, targeted therapies, and experimental research.
MRI Procedure:
The MRI (Magnetic Resonance Imaging) procedure is a non-invasive medical imaging technique used to visualize the internal structures of the body. Here’s an overview of the typical steps involved in an MRI procedure:
1. Scheduling and Preparation:
- Patients are scheduled for an MRI appointment, and they receive instructions regarding any specific preparations they need to follow.
- Patients may be asked to fast before certain types of MRI scans, especially those involving the abdomen or pelvis. They should also avoid wearing metallic objects, such as jewelry and clothing with metal zippers or snaps.
2. Check-In:
- Patients arrive at the MRI facility and check in at the reception or imaging department.
3. Changing into a Gown:
- To avoid interference with the MRI’s magnetic field, patients may be asked to change into a gown provided by the facility. Any metallic objects, such as watches or piercings, should be removed.
4. Screening for Safety:
- Patients undergo a safety screening to check for any metal objects within the body, as these can pose safety risks in the MRI environment.
- The technologist will ask about allergies to contrast agents and any prior adverse reactions to them.
5. Placement on the MRI Table:
- Patients are positioned on the MRI table, either lying down or in a specific position depending on the area being imaged.
- It’s essential for patients to remain as still as possible during the scan to prevent motion artifacts.
6. Intravenous (IV) Line:
- If a contrast agent (gadolinium-based) is required for the MRI, an IV line may be inserted into the patient’s arm. The contrast agent is typically administered through the IV during the scan.
7. Ear Protection:
- Patients are provided with earplugs or headphones to protect their hearing from the loud knocking or thumping noises the MRI machine makes during the scan.
8. Entering the MRI Machine:
- The MRI technologist will guide the patient into the MRI machine, which is a large, tunnel-like structure. Some MRI machines are open or wide-bore, which can be more comfortable for patients who are claustrophobic.
9. Communicating with the Technologist:
- Patients are in constant communication with the technologist through an intercom system. They can ask questions, express concerns, or request assistance if needed.
10. MRI Scanning:
- The MRI machine generates a series of images or slices of the body part under examination.
- Scans can last from a few minutes to over an hour, depending on the type of MRI and the area being imaged.
- Patients are required to remain still during the scans to obtain clear images.
- Some MRI scans may involve breath-holding instructions for certain sequences.
11. Contrast Injection (if applicable):
- If contrast is needed, the technologist will administer it through the IV line during specific sequences of the scan.
12. Completion and Exit:
- Once the MRI scan is complete, the technologist will guide the patient out of the machine.
- Patients can change back into their regular clothing and collect their belongings.
13. Post-Procedure Instructions:
- Depending on the use of contrast agents and individual patient requirements, there may be specific post-procedure instructions provided.
14. Image Interpretation:
- A radiologist will interpret the MRI images, and the results will be sent to the referring physician, who will discuss the findings with the patient.
MRI Interpretation:
Interpreting MRI (Magnetic Resonance Imaging) images is a complex process that requires specialized training and expertise. Radiologists, who are medical doctors with specialized training in medical imaging, are primarily responsible for interpreting MRI scans. Here’s an overview of the MRI interpretation process:
- Image Review:
- The radiologist begins by reviewing the series of MRI images obtained during the scan. These images are typically stored digitally.
- Clinical Information:
- The radiologist considers the clinical information provided by the referring physician, including the patient’s medical history, symptoms, and the reason for the MRI.
- Image Sequences:
- MRI scans often include multiple sequences, each designed to highlight different aspects of the anatomy or pathology. The radiologist evaluates all relevant sequences.
- Anatomy Assessment:
- The radiologist identifies and assesses the normal anatomy and structures in the region of interest. This includes evaluating the brain, spinal cord, organs, blood vessels, bones, and soft tissues, depending on the area being imaged.
- Pathological Findings:
- The radiologist looks for abnormalities, such as tumors, lesions, inflammation, hemorrhage, or other pathological conditions, and characterizes their size, location, and characteristics.
- Contrast Enhancement:
- If a contrast agent (gadolinium-based) was administered during the MRI, the radiologist assesses the enhancement patterns of tissues and lesions to provide additional diagnostic information.
- Comparison Studies:
- In some cases, the radiologist may compare the current MRI images with prior MRI scans, X-rays, CT scans, or other imaging studies to track changes over time.
- Functional Imaging:
- If functional MRI (fMRI) or spectroscopy (MRS) was performed, the radiologist analyzes the functional data or chemical composition of tissues to assess brain function or metabolic activity.
- Report Generation:
- The radiologist generates a comprehensive written report summarizing their findings. This report includes a description of normal and abnormal findings, a differential diagnosis (if applicable), and any recommended follow-up studies.
- Communication with Referring Physician:
- The radiologist communicates the results of the MRI interpretation to the referring physician, who then discusses the findings with the patient and determines the next steps, such as treatment or further diagnostic tests.
- Quality Assurance:
- Quality control and assurance procedures are in place to ensure the accuracy and reliability of MRI interpretations. Radiology departments often have protocols and peer review processes to maintain high standards.
Special Considerations:
Special considerations in Magnetic Resonance Imaging (MRI) encompass a range of factors that may affect the MRI procedure or require additional attention. These considerations can relate to specific patient populations, medical conditions, or unique circumstances. Here are some important special considerations in MRI:
- Pediatric Patients:
- MRI protocols for children often involve age-appropriate techniques, sedation options, and child-friendly environments to minimize anxiety and ensure cooperation during the scan.
- Geriatric Patients:
- Older patients may have mobility issues or comorbidities that require special attention during positioning and comfort considerations.
- Pregnancy:
- MRI is generally considered safe during pregnancy, especially after the first trimester. However, it is crucial to minimize the use of contrast agents and ensure patient comfort and safety.
- Claustrophobia:
- Patients with claustrophobia may require additional support, such as pre-scan counseling, sedation, or the use of open-bore or wide-bore MRI machines to reduce anxiety.
- Metal Implants and Devices:
- Patients with certain metallic implants or devices (e.g., pacemakers, cochlear implants, aneurysm clips) may not be eligible for MRI or may require specialized, MRI-compatible devices.
- Renal Function:
- Patients with impaired renal function must be carefully evaluated before receiving gadolinium-based contrast agents, as there is a risk of nephrogenic systemic fibrosis (NSF).
- Allergies:
- Patients with known allergies, particularly to contrast agents, should be thoroughly assessed and receive appropriate pre-medication or alternative imaging methods if necessary.
- Anesthesia or Sedation:
- Some patients, especially children and individuals with severe anxiety, may require sedation or anesthesia to ensure they remain still during the MRI.
- Emergency and Life Support Equipment:
- MRI suites must be equipped with MRI-safe emergency equipment, including resuscitation and defibrillation devices.
- Research and Specialized Protocols:
- Research MRI studies may involve unique protocols, including advanced imaging techniques or contrast agents designed for specific research purposes.
- Limited Mobility or Disabilities:
- Patients with limited mobility or physical disabilities may require customized positioning or assistance to ensure their comfort and safety during the scan.
- Patient Communication:
- Patients who may have difficulty communicating, such as those with cognitive impairments or language barriers, may need additional support and clear communication strategies.
- Chemical Sensitivities:
- Patients with sensitivities to the scents or materials in the MRI suite may require accommodations to minimize discomfort or allergic reactions.
- Emergency Planning:
- MRI facilities should have well-established emergency protocols and procedures, including the ability to quickly remove a patient from the scanner in case of an emergency.
Limitations and Considerations:
- Metal Interference: MRI can be affected by metallic objects in or on the body, limiting its use for patients with certain implants or metal fragments.
- Claustrophobia and Anxiety: The enclosed MRI machine can trigger claustrophobia and anxiety in some patients, necessitating open or wide-bore machines or sedation.
- Scan Duration: MRI scans can be lengthy, requiring patient cooperation for extended periods.
- Motion Artifacts: Patient movement can degrade image quality, necessitating stillness during scans.
- Cost: MRI procedures can be expensive for both healthcare facilities and patients.
- Limited Access: Not all healthcare facilities have MRI machines, limiting patient access to this imaging modality.
- Noise: MRI machines produce loud noises during scans, which can be discomforting for patients.
- Gadolinium Contrast: Concerns about gadolinium retention in the body have prompted safety considerations when using contrast agents.
- Tissue Limitations: MRI may not be the optimal choice for imaging certain tissues or pathologies.
- Contraindications: Specific medical conditions or circumstances may contraindicate MRI, including severe claustrophobia and incompatible metallic objects.
- Availability of Specialized Sequences: Not all MRI facilities may offer specialized imaging sequences or advanced techniques.
- Operator Dependence: The quality of MRI images and diagnostic accuracy can depend on the skill and expertise of healthcare professionals.
Advantages and Disadvantages:
Magnetic Resonance Imaging (MRI) is a valuable medical imaging modality with several advantages and disadvantages:
Advantages:
- Non-Invasive: MRI does not use ionizing radiation, making it a safe imaging method for repeated use without significant health risks.
- Excellent Soft Tissue Contrast: MRI provides superb contrast between different types of soft tissues, making it ideal for visualizing organs, muscles, nerves, and tumors.
- Multi-Planar Imaging: MRI allows for imaging in multiple planes (axial, sagittal, coronal) without repositioning the patient, providing a comprehensive view of anatomical structures.
- No Radiation Exposure: Unlike X-ray and CT scans, MRI does not expose patients to ionizing radiation, making it suitable for vulnerable populations, such as pregnant women and children.
- Functional Imaging: Functional MRI (fMRI) can capture real-time images of brain activity, aiding in the study of brain functions and disorders.
- Excellent Brain Imaging: MRI is the gold standard for brain imaging, providing detailed views of brain structures and abnormalities.
- Contrast Enhancement: The use of contrast agents (e.g., gadolinium) can enhance the visibility of specific tissues or blood vessels.
- No Known Long-Term Health Risks: MRI has no known long-term health risks associated with its use.
Disadvantages:
- High Cost: MRI equipment and maintenance are expensive, leading to higher healthcare costs for patients and healthcare facilities.
- Limited Availability: Not all medical facilities have access to MRI machines, potentially limiting patient access to this imaging modality.
- Long Scan Times: MRI scans can be time-consuming, especially for some types of examinations, which can be uncomfortable for patients.
- Claustrophobia: The enclosed MRI machine can induce claustrophobia and anxiety in some individuals, necessitating open-bore or wide-bore MRI machines.
- Motion Sensitivity: MRI is sensitive to patient motion, and even small movements can result in motion artifacts and reduced image quality.
- Metallic Interference: MRI can be affected by metallic objects in or on the body, potentially limiting its use in patients with certain implants or metal fragments.
- Contrast Allergies: Some patients may be allergic to contrast agents, which can lead to adverse reactions.
- Less Effective for Certain Tissues: MRI may not be the best choice for imaging certain tissues, such as bones or lungs, for which other modalities like X-ray or CT scans may be more suitable.
- Operator Dependence: The quality of MRI images and diagnostic accuracy can depend on the skill and expertise of healthcare professionals.
- Contraindications: Specific medical conditions or circumstances may contraindicate MRI, such as severe claustrophobia, the presence of incompatible metallic objects, or certain medical implants.
Advancements in MRI Technology:
- Higher Field Strength Magnets: The development of stronger magnets, including 3T and 7T MRI systems, has improved image resolution and allowed for more detailed anatomical and functional imaging.
- Faster Imaging Techniques: Advanced pulse sequences and parallel imaging techniques have reduced scan times, making MRI more comfortable for patients and improving clinical throughput.
- Wide-Bore and Open MRI Machines: These designs address claustrophobia concerns and accommodate larger or immobile patients.
- Functional MRI (fMRI): fMRI has become a powerful tool for mapping brain activity and understanding cognitive processes, such as memory, language, and emotion.
- Diffusion Tensor Imaging (DTI): DTI provides insights into white matter tracts in the brain, enabling the study of neurological disorders and connectivity between brain regions.
- Perfusion Imaging: Techniques like arterial spin labeling (ASL) allow for non-contrast evaluation of tissue perfusion, aiding in stroke assessment and brain tumor characterization.
- Multinuclear MRI: Beyond hydrogen, MRI can now be performed using other nuclei like carbon-13, fluorine-19, and sodium-23, opening new avenues for metabolic and functional studies.
- Functional Connectivity MRI (fcMRI): This technique examines correlations in activity between different brain regions and contributes to the understanding of brain networks.
- Quantitative MRI: Methods like MR spectroscopy and relaxometry provide quantitative data on tissue properties, aiding in disease characterization and monitoring.
- Cardiac MRI: Improved cardiac imaging techniques, including cine MRI and 4D flow MRI, enhance the assessment of heart function, blood flow, and myocardial tissue.
- MRI-guided Interventions: Real-time MRI guidance is used in minimally invasive procedures, such as biopsies and tumor ablations, improving accuracy and safety.
- Artificial Intelligence (AI) and Machine Learning: AI algorithms assist in image analysis, automated lesion detection, and predicting disease outcomes, reducing the burden on radiologists and enhancing diagnostic accuracy.
- Advanced Coil Technology: Specialized coils, including phased-array and surface coils, optimize image quality for specific anatomical regions.
- MR Elastography: This technique measures tissue stiffness and is used in liver fibrosis assessment and cancer diagnosis.
- Advanced Contrast Agents: Development of novel contrast agents, including molecular imaging agents, enhances tissue characterization and detection of specific biomarkers.
- 3D and 4D Imaging: High-resolution 3D and dynamic 4D imaging sequences provide detailed anatomical and functional information.
- Pediatric and Neonatal MRI: Tailored imaging protocols and techniques improve the use of MRI in pediatric and neonatal populations.
- Hybrid Imaging: Combining MRI with other modalities like positron emission tomography (PET) or single-photon emission computed tomography (SPECT) offers complementary information for diagnosis and treatment planning.
FAQs:
What is MRI?
MRI is a non-invasive medical imaging technique that uses strong magnets and radio waves to create detailed images of the body’s internal structures.
How does MRI work?
MRI works by aligning the hydrogen atoms in the body’s tissues with a magnetic field. When radio waves are applied, these atoms emit signals that are used to create images.
Is MRI safe?
Generally, MRI is considered safe because it does not use ionizing radiation. However, it may not be safe for patients with certain metallic implants or devices.
How long does an MRI scan take?
The duration of an MRI scan varies depending on the type of scan and the area being imaged. It can range from a few minutes to over an hour.
Do I need to prepare for an MRI?
Preparation requirements may vary, but patients are often advised to remove metallic objects, follow fasting instructions (for abdominal scans), and wear loose-fitting, non-metallic clothing.
Can I eat or drink before an MRI?
It depends on the specific scan. Some MRI scans, such as those involving the abdomen, may require fasting for several hours before the procedure.
Is contrast used in MRI?
Contrast agents, such as gadolinium, can be used to enhance the visibility of certain tissues or blood vessels in MRI scans.
Are there any risks associated with MRI contrast agents?
While rare, some patients may experience allergic reactions to contrast agents. It’s important to inform the healthcare provider of any known allergies.
Can I have an MRI if I’m pregnant?
MRI is generally considered safe during pregnancy, especially after the first trimester. However, the use of contrast agents is typically minimized during pregnancy.
What should I expect during an MRI scan?
During the scan, you will lie on a table that slides into the MRI machine. You’ll need to remain as still as possible to obtain clear images.
Is MRI loud?
Yes, MRI machines produce loud knocking or thumping noises during the scan. Patients are provided with ear protection to minimize noise exposure.
Can I have an MRI if I’m claustrophobic?
Open or wide-bore MRI machines are available for individuals with claustrophobia. Some patients may also receive sedation to help with anxiety.
What can an MRI diagnose?
MRI can diagnose a wide range of medical conditions, including brain disorders, musculoskeletal injuries, tumors, vascular issues, and more.
Do I get MRI results immediately?
Typically, MRI results are not provided immediately. A radiologist interprets the images and sends a report to the referring physician, who will discuss the findings with you.
Are there any contraindications for MRI?
Yes, certain medical conditions or the presence of incompatible metallic objects may contraindicate MRI. It’s essential to inform your healthcare provider of any relevant factors.
Conclusion:
In conclusion, Magnetic Resonance Imaging (MRI) is a vital and versatile medical imaging technology that offers several advantages, such as excellent soft tissue contrast, non-invasiveness, and absence of ionizing radiation. It has a wide range of clinical applications across various medical specialties and continues to evolve with advancements in technology.
However, there are important considerations and limitations associated with MRI, including the need to address metal interference, manage patient claustrophobia and anxiety, and deal with long scan times. Additionally, MRI can be costly, and access to this imaging modality may be limited in some areas.