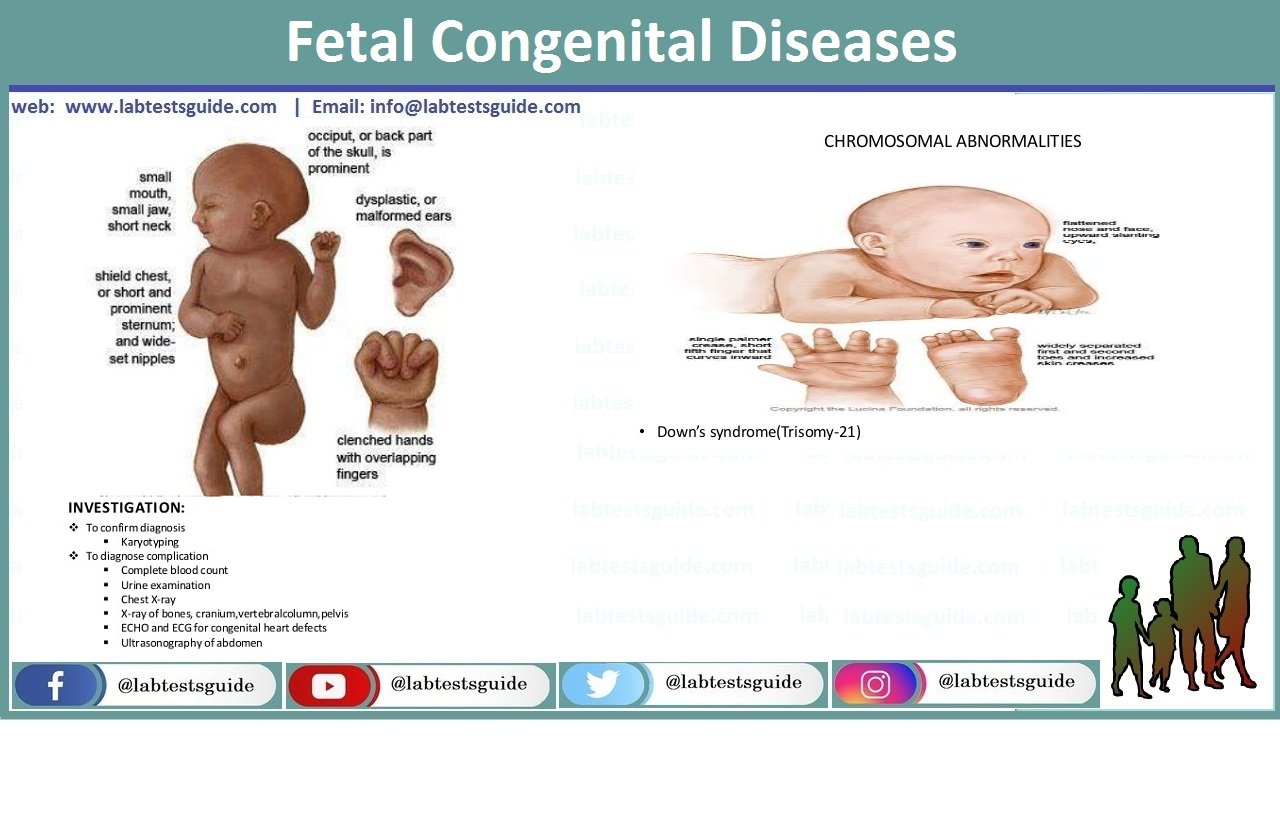
Congenital disorders can be defined as structural or functional anomalies that occur during intrauterine life. Also called birth defects, congenital anomalies or congenital malformations, these conditions develop prenatally and may be identified before or at birth, or later in life.
Definition of Fetal Congenital Conditions.
“Fetal congenital conditions,” often referred to as “congenital anomalies” or “birth defects,” are structural or functional abnormalities present in a baby at birth. These conditions can affect various parts of the body, including organs, tissues, and body systems, and they may result from genetic factors, environmental influences, or a combination of both. Fetal congenital conditions can range from mild to severe and may have lifelong implications for the affected individual’s health and well-being.
Causes and Risk Factors:
Genetic Factors:
- Inherited Genetic Mutations: Some congenital conditions are caused by specific gene mutations that are passed down from parents to their children. Examples include cystic fibrosis, sickle cell anemia, and muscular dystrophy.
- Chromosomal Abnormalities: Conditions like Down syndrome, Edwards syndrome, and Patau syndrome result from chromosomal abnormalities, where there is an extra or missing chromosome.
Environmental Factors:
- Maternal Exposure to Teratogens: Teratogens are substances that can disrupt fetal development and lead to congenital conditions when a pregnant woman is exposed to them. Examples include alcohol, tobacco, certain medications, and illicit drugs.
- Maternal Infections: Some infections during pregnancy, such as rubella (German measles), cytomegalovirus (CMV), and Zika virus, can cause congenital conditions when the fetus is infected in utero.
- Radiation and Environmental Toxins: Exposure to high levels of ionizing radiation or environmental toxins, like lead or mercury, can increase the risk of birth defects.
Lifestyle Factors:
- Maternal Nutrition: Inadequate maternal nutrition, particularly a deficiency in folic acid, can increase the risk of neural tube defects.
- Maternal Age: Advanced maternal age (over 35 years) is associated with an increased risk of certain congenital conditions, such as Down syndrome.
- Maternal Health: Chronic maternal conditions like diabetes or obesity can contribute to an elevated risk of congenital anomalies.
Random Mutations: In some cases, congenital conditions occur due to random mutations that happen during fetal development. These are not inherited but rather arise spontaneously.- Family History: A family history of congenital conditions may increase the risk of having a child with a similar condition, especially if there is a known genetic component.
- Multiple Factors: Often, it’s not a single factor but a combination of genetic predisposition and environmental exposures that contribute to congenital conditions. For example, a genetic predisposition for heart defects combined with maternal smoking during pregnancy can increase the risk of congenital heart defects.
Sign and Symptoms of Fetal Congenital :
Here are some common signs and symptoms associated with fetal congenital conditions.
Physical Abnormalities:
- Malformed Limbs: Conditions like limb reduction defects can result in missing or underdeveloped limbs.
- Cleft Lip and Palate: Babies may have a gap or split in the upper lip (cleft lip), the roof of the mouth (cleft palate), or both.
- Facial Dysmorphism: Some congenital conditions can lead to distinct facial features, such as those seen in Down syndrome.
Cardiovascular Symptoms:
- Cyanosis: Bluish discoloration of the skin and lips, indicating poor oxygenation in congenital heart defects.
- Tachypnea: Rapid breathing due to heart-related issues.
Respiratory Symptoms:
- Respiratory Distress: Difficulty breathing, rapid breathing, or grunting sounds during breathing may occur in babies with certain lung or diaphragm anomalies.
Neurological Signs:
- Seizures: Some congenital brain abnormalities can lead to seizures in newborns.
- Developmental Delays: Delays in achieving developmental milestones, such as rolling over, sitting up, or crawling, may be observed.
Gastrointestinal Symptoms:
- Feeding Difficulties: Difficulty with sucking, swallowing, or digesting milk or formula.
- Vomiting: Frequent vomiting, which could be related to gastrointestinal anomalies.
Genitourinary Manifestations:
- Abnormal Urination: Difficulty urinating, blood in the urine, or other urinary issues.
- Ambiguous Genitalia: In some cases, babies may be born with genitalia that do not clearly appear male or female.
Skeletal and Muscular Abnormalities:
- Joint Contractures: Inability to fully extend or move joints due to musculoskeletal issues.
- Scoliosis: Curvature of the spine, which may be present in certain congenital conditions.
Metabolic and Endocrine Signs:
Failure to Thrive: Inadequate weight gain and growth.
Hypoglycemia: Low blood sugar levels in some metabolic disorders.
Hearing and Vision Problems:
Hearing Loss: Partial or complete hearing loss may occur.
Vision Impairment: Congenital conditions can lead to visual impairments, including blindness.
Diagnosis and Prenatal Screening:
Prenatal Screening:
These tests are non-invasive and do not pose a significant risk to the fetus. Some common prenatal screening tests include.
- Maternal Blood Tests: These tests measure specific markers in the mother’s blood to assess the risk of certain chromosomal abnormalities, such as Down syndrome (Trisomy 21), Edwards syndrome (Trisomy 18), and neural tube defects.
- First-Trimester Combined Screening: This combines a maternal blood test (serum screening) with a nuchal translucency ultrasound scan performed between 11 and 14 weeks of gestation. It assesses the risk of Down syndrome and other chromosomal abnormalities.
- Quadruple Screen or Quad Marker Screening: Performed between the 15th and 20th weeks of pregnancy, this blood test assesses the risk of neural tube defects and some chromosomal conditions. It measures alpha-fetoprotein (AFP), human chorionic gonadotropin (hCG), estriol, and inhibin A.
- Cell-Free DNA Testing (Non-Invasive Prenatal Testing or NIPT): This advanced blood test analyzes fetal DNA circulating in the mother’s bloodstream to screen for common chromosomal abnormalities, such as Down syndrome, with high accuracy.
- Ultrasound Scans: Routine ultrasound examinations can provide valuable information about the developing fetus’s anatomy and growth. Certain structural anomalies may be detected through ultrasound, although it may not identify all congenital conditions.
Prenatal Diagnosis:
Common prenatal diagnostic tests include.
- Amniocentesis: During this procedure, a sample of amniotic fluid is extracted through a thin needle inserted into the uterus. Amniocentesis can diagnose chromosomal abnormalities, neural tube defects, and certain genetic conditions.
- Chorionic Villus Sampling (CVS): CVS involves the removal of a small sample of placental tissue (chorionic villi) for genetic testing. It is typically performed between 10 and 13 weeks of pregnancy and can detect chromosomal abnormalities and genetic conditions.
- Fetal MRI: In some cases, a magnetic resonance imaging (MRI) scan may be used to provide detailed images of the fetus’s anatomy, particularly if ultrasound results are inconclusive or further clarification is needed.
Prevention and Genetic Counseling:
Prevention:
Preconception Planning: Key steps in preconception planning include:
- Genetic Testing: Individuals or couples with a family history of genetic conditions may undergo genetic testing to assess their risk of passing on these conditions to their offspring.
- Medication Review: Reviewing medications and discussing potential risks with a healthcare provider to avoid teratogenic drugs (drugs that can harm fetal development) during pregnancy.
- Folic Acid Supplementation: Adequate folic acid intake before and during early pregnancy can reduce the risk of neural tube defects.
- Prenatal Care: Early and consistent prenatal care is essential to monitor the health and development of the fetus. Regular check-ups, screenings, and ultrasounds help identify potential issues early and provide opportunities for intervention and treatment.
Genetic Counseling:
- Risk Assessment: Genetic counselors assess an individual or couple’s risk of having a child with a congenital condition based on family medical history, genetic testing, and other relevant factors.
- Education: Genetic counselors educate individuals and couples about the specific genetic conditions they may be at risk for, the inheritance patterns, and the likelihood of having an affected child.
- Informed Decision-Making: Genetic counseling helps individuals make informed decisions about family planning, including options such as preimplantation genetic diagnosis (PGD), adoption, or the use of assisted reproductive technologies.
- Prenatal Testing: If indicated, genetic counselors can facilitate and interpret prenatal screening and diagnostic tests, such as amniocentesis or chorionic villus sampling, to provide accurate information about the fetus’s health.
- Emotional Support: Coping with the possibility or reality of a congenital condition can be emotionally challenging. Genetic counselors offer emotional support and connect individuals and families with appropriate resources and support groups.
- Family Communication: Genetic counseling can assist individuals in discussing genetic risks and congenital conditions within their families and help facilitate important conversations.
- Advocacy: Genetic counselors can advocate for their clients by helping them access appropriate medical care and ensuring that their wishes and values are considered in medical decision-making.
Treatment and Management:
Here are some key aspects of treatment and management.
Medical Interventions:
Surgery: Many congenital conditions require surgical intervention to correct structural abnormalities or improve function. For example, congenital heart defects, cleft lip and palate, and limb abnormalities often require surgical procedures.
Medications: Some congenital conditions can be managed with medications to control symptoms, reduce complications, or address underlying issues. For instance, medications can help manage seizures in individuals with certain neurological conditions.
Pain Management: For conditions associated with chronic pain, pain management strategies may be employed to enhance the individual’s comfort and well-being.
Nutritional Support: Babies born with certain congenital conditions, such as feeding difficulties or gastrointestinal anomalies, may require specialized feeding methods or nutritional support.
Early Intervention Programs:
- Physical Therapy: Physical therapy can help individuals with musculoskeletal or mobility issues improve their physical function and quality of life.
- Occupational Therapy: Occupational therapy aims to improve daily living skills and independence for individuals with physical or developmental challenges.
- Speech Therapy: For conditions affecting speech and language development, speech therapy can be beneficial.
- Developmental Support: Early intervention programs can provide support to infants and young children with developmental delays or disabilities to help them reach their developmental milestones.
Supportive Care:
- Psychological Support: Individuals and families affected by congenital conditions may benefit from psychological counseling or therapy to cope with emotional challenges and stress.
- Support Groups: Joining support groups for families and individuals dealing with similar conditions can provide valuable emotional support and a sense of community.
- Educational Services: Children with congenital conditions may require special education services tailored to their needs.
Ongoing Monitoring:
- Regular Check-ups: Individuals with congenital conditions often require lifelong medical follow-up to monitor their health and address any emerging issues.
- Prenatal Care: For some congenital conditions, prenatal care may be provided for expectant mothers to optimize fetal health and prepare for any necessary interventions after birth.
Assistive Devices and Technology:
- Orthopedic Devices: Orthopedic braces, prosthetics, or mobility aids may be prescribed to improve mobility and function.
- Hearing Aids and Cochlear Implants: These devices can help individuals with hearing impairments communicate effectively.
- Communication Devices: Augmentative and alternative communication (AAC) devices can assist individuals with speech or language difficulties.
Genetic Counseling and Family Planning:
- Genetic Counseling: Families affected by congenital conditions may benefit from genetic counseling to understand the genetic basis of the condition and make informed family planning decisions.
Palliative Care and End-of-Life Care:
- For some severe congenital conditions with a limited life expectancy, palliative care and end-of-life care may be provided to ensure comfort and dignity.
Common Fetal Congenital Conditions:
Some of the most common fetal congenital conditions include.
- Congenital Heart Defects: These are structural abnormalities in the heart’s chambers, valves, or blood vessels. Examples include atrial septal defects, ventricular septal defects, and Tetralogy of Fallot.
- Neural Tube Defects (NTDs): NTDs are a group of conditions that affect the development of the brain and spinal cord. The most well-known NTD is spina bifida, which involves incomplete closure of the spinal column.
- Cleft Lip and Palate: These are facial deformities that occur when the tissues forming the lip and palate do not fully come together during fetal development, leading to an opening or gap.
- Down Syndrome (Trisomy 21): Down syndrome is a chromosomal disorder caused by the presence of an extra copy of chromosome 21. It is characterized by intellectual disabilities, distinctive facial features, and various health issues.
- Chromosomal Abnormalities: Conditions like Edwards syndrome (Trisomy 18) and Patau syndrome (Trisomy 13) result from extra copies of chromosomes 18 and 13, respectively. These conditions are associated with severe developmental and medical challenges.
- Cystic Fibrosis: This is an inherited genetic disorder that affects the respiratory, digestive, and reproductive systems. It results in thick, sticky mucus production that can lead to breathing difficulties and digestive problems.
- Clubfoot: Clubfoot is a musculoskeletal condition in which a baby’s foot is twisted or turned inward. It can affect one or both feet.
- Hydrocephalus: This condition involves the accumulation of cerebrospinal fluid in the brain, leading to increased intracranial pressure. It may require surgical intervention to drain excess fluid.
- Sickle Cell Disease: Sickle cell disease is a genetic blood disorder that causes abnormal, crescent-shaped red blood cells. It can result in anemia, pain crises, and organ damage.
- Hypoplastic Left Heart Syndrome (HLHS): HLHS is a severe congenital heart defect in which the left side of the heart is underdeveloped, making it difficult to pump blood effectively.
- Gastroschisis: This condition involves a hole in the abdominal wall through which the intestines protrude. Surgical repair is typically required after birth.
- Cerebral Palsy: Cerebral palsy is a group of neurological disorders that affect muscle coordination and movement. It can result from brain damage during fetal development or birth.
- Fetal Alcohol Spectrum Disorders (FASD): These conditions result from prenatal alcohol exposure and can cause a range of physical, cognitive, and behavioral impairments.
- Turner Syndrome: Turner syndrome is a genetic condition in which females have only one fully functioning X chromosome instead of the usual two. It leads to various physical and developmental challenges.
- Diaphragmatic Hernia: This occurs when there is a hole or weak spot in the diaphragm, allowing abdominal organs to enter the chest cavity and compress the lungs. It can cause breathing difficulties.
Impact on Families:
Here are some of the ways in which congenital conditions can affect families.
Emotional and Psychological Impact:
- Shock and Grief: Learning about a congenital condition in their child can be emotionally overwhelming for parents. It may evoke feelings of shock, grief, and sadness as they adjust to the diagnosis.
- Anxiety and Stress: Parents often experience ongoing anxiety and stress related to the health and future of their child. Frequent medical appointments, treatments, and surgeries can add to this burden.
- Depression: Coping with a congenital condition can lead to parental depression or feelings of helplessness, especially if they perceive limited support or understanding from others.
- Stigma: Some families may face social stigma or judgment from others, which can compound emotional distress.
Financial Impact:
- Medical Expenses: Congenital conditions may result in significant medical expenses, including surgeries, therapies, medications, and assistive devices.
- Reduced Income: Caring for a child with complex medical needs may require parents to reduce their work hours or stop working altogether, impacting the family’s income.
- Insurance Challenges: Families may encounter difficulties in securing and affording health insurance coverage for their child’s specific medical needs.
Changes in Daily Life:
- Time Commitment: Managing medical appointments, therapies, and caregiving responsibilities can consume a significant amount of a family’s time.
- Altered Family Dynamics: The needs of a child with a congenital condition can shift family roles and dynamics. Siblings may experience feelings of neglect or jealousy.
- Isolation: Families may become socially isolated due to the demands of caring for their child and concerns about their child’s health in public settings.
Navigating the Healthcare System:
- Complex Medical Care: Coordinating care and advocating for the best possible treatment for a child with a congenital condition can be challenging and time-consuming.
- Healthcare Decisions: Families may face difficult decisions about treatment options, surgeries, and interventions, which can be emotionally taxing.
Support Systems:
- Support Groups: Many families find comfort and guidance by connecting with other parents facing similar challenges through support groups.
- Professional Counseling: Access to mental health services can help parents and family members manage the emotional impact of the condition.
- Advocacy Organizations: Various organizations offer resources, information, and advocacy support for families dealing with congenital conditions.
Relationship Strain:
- Marital and Family Relationships: The stress and demands of caring for a child with a congenital condition can strain marital and family relationships. It’s important for parents to communicate openly and seek support when needed.
- Siblings: Siblings may experience a range of emotions, including jealousy, guilt, and concern for their affected sibling.
Medical Advances and Research:
Here are some key areas of progress and research in this field.
Prenatal Diagnosis and Screening:
- Advanced Imaging: The development of advanced imaging techniques, such as 3D and 4D ultrasound, fetal magnetic resonance imaging (MRI), and high-resolution fetal echocardiography, allows for more detailed and accurate prenatal diagnosis of congenital conditions.
- Non-Invasive Prenatal Testing (NIPT): NIPT, which analyzes cell-free fetal DNA in maternal blood, has improved the accuracy of prenatal screening for chromosomal abnormalities and certain genetic conditions.
Genetic Research:
- Genomic Sequencing: Advances in genomic sequencing technologies have led to a deeper understanding of the genetic basis of congenital conditions, enabling more precise diagnoses and personalized treatment approaches.
- Gene Therapy: Research into gene therapy holds promise for treating some genetic-based congenital conditions by correcting or replacing defective genes.
Surgical Techniques:
- Minimally Invasive Surgery: Minimally invasive surgical techniques, including fetal surgery, have been developed to address congenital conditions such as spina bifida, congenital diaphragmatic hernia, and twin-twin transfusion syndrome (TTTS).
- 3D Printing: 3D printing technology is used to create customized surgical models and implants for complex procedures.
Regenerative Medicine:
- Stem Cell Therapies: Research in stem cell therapies is exploring the potential to repair or regenerate damaged tissues and organs affected by congenital conditions.
- Tissue Engineering: Advances in tissue engineering are being applied to create functional replacement tissues and organs for congenital anomalies.
Drug Development:
- Pharmacological Treatments: Ongoing research seeks to develop pharmaceutical interventions to manage and treat congenital conditions, such as genetic disorders and metabolic disorders.
- Clinical Trials: Clinical trials are conducted to test the safety and efficacy of potential new treatments for congenital conditions.
Fetal Medicine and Intervention:
- In Utero Interventions: Continued research is exploring the safety and effectiveness of in utero interventions for congenital conditions, including surgeries and treatments before birth.
- Fetal Monitoring: Advances in fetal monitoring technologies, such as fetal electrocardiography and fetal MRI, are improving the assessment and management of fetal health.
Preventive Measures:
- Folic Acid Supplementation: Public health campaigns and education on the importance of folic acid supplementation before and during pregnancy have helped reduce the incidence of neural tube defects.
- Teratogen Awareness: Increased awareness about the risks of teratogenic substances (substances that can harm fetal development) has led to improved avoidance measures during pregnancy.
- Telemedicine and Telehealth: The integration of telemedicine and telehealth services has improved access to medical expertise and consultations for families living in remote or underserved areas.
- Data Sharing and Collaboration: International collaboration and the sharing of research data have accelerated progress in understanding the causes and outcomes of congenital conditions.
- Patient and Family Advocacy: Advocacy organizations and support groups for families affected by congenital conditions play a vital role in raising awareness, funding research, and promoting policy changes to benefit affected individuals and families.
FAQs:
What are fetal congenital conditions?
Fetal congenital conditions, also known as birth defects or congenital anomalies, are structural or functional abnormalities present in a baby at birth. They can affect various parts of the body and may result from genetic factors, environmental influences, or a combination of both.
How are fetal congenital conditions diagnosed during pregnancy?
Prenatal screening tests, such as maternal blood tests and ultrasounds, can assess the risk of certain congenital conditions. If indicated, further diagnostic tests like amniocentesis or chorionic villus sampling (CVS) can provide a definitive diagnosis.
Can congenital conditions be prevented?
Some congenital conditions can be prevented or their risk minimized through preconception planning, genetic counseling, avoiding teratogenic substances during pregnancy, and adequate prenatal care.
What are common types of congenital conditions?
Common congenital conditions include congenital heart defects, neural tube defects (e.g., spina bifida), cleft lip and palate, Down syndrome, and limb abnormalities. However, there are many different types of congenital conditions.
How are congenital conditions treated?
Treatment varies depending on the type and severity of the condition but may include surgery, medications, therapies (e.g., physical therapy, speech therapy), assistive devices, and ongoing medical care.
What is genetic counseling, and who should consider it?
Genetic counseling is a service provided by trained professionals to assess an individual or family’s risk of inherited genetic conditions. It’s recommended for individuals or couples with a family history of genetic conditions, recurrent miscarriages, or concerns about the risk of having a child with a congenital condition.
Are there support networks for families dealing with congenital conditions?
Yes, there are many support groups and advocacy organizations that provide information, resources, and emotional support for individuals and families affected by congenital conditions. These organizations can help connect families with others facing similar challenges.
What are the latest medical advances in the field of congenital conditions?
Recent medical advances include advancements in prenatal diagnosis, genetic research, surgical techniques, stem cell therapies, and regenerative medicine, all aimed at improving the understanding and management of congenital conditions.
How can I find specialized care for my child with a congenital condition?
Specialized care is typically available at children’s hospitals or medical centers with specialized pediatric services. Seeking referrals from your primary care provider or genetic counselor can help you find the appropriate care for your child.
Is there ongoing research into congenital conditions?
Yes, ongoing research continues to advance our understanding of congenital conditions and develop new treatments and interventions. Collaborative efforts among researchers, healthcare providers, and advocacy groups drive progress in this field.
Conclusion:
In conclusion, fetal congenital conditions are a diverse group of structural or functional abnormalities present at birth, and they can have a significant impact on affected individuals and their families. Advances in medical science, prenatal diagnosis, surgical techniques, and ongoing research offer hope for improved outcomes and quality of life for those living with these conditions. Early diagnosis, access to specialized care, genetic counseling, and strong support networks play pivotal roles in addressing the challenges associated with congenital conditions. While the journey can be challenging, the resilience of affected individuals and the unwavering support of their families and communities demonstrate the remarkable capacity to adapt, overcome, and thrive in the face of adversity.