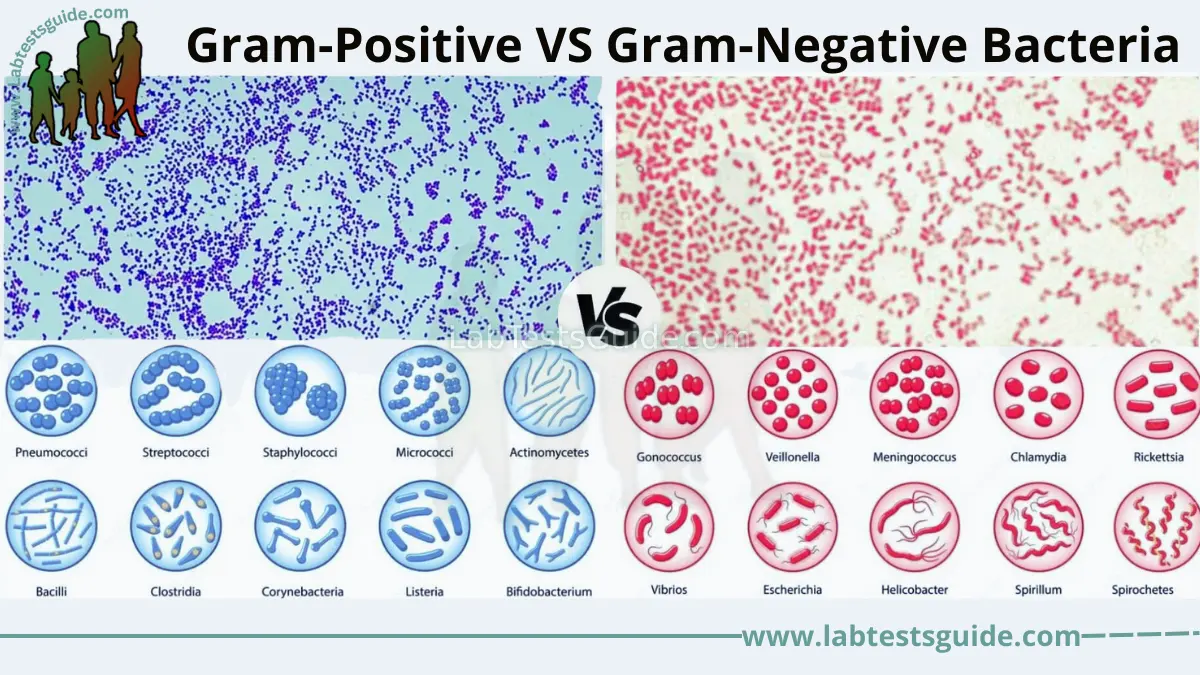
Gram-Positive vs Gram-Negative Bacteria
Bacteria are ubiquitous microorganisms that inhabit nearly every environment on Earth. While they may appear similar under a basic microscope, their structural anatomy dictates how they survive, cause disease, and react to life-saving medications. Explore the definitive comparison guide below.
Gram Stain Result
Positive retains Purple dye. Negative turns Pink/Red.
Cell Wall Structure
Positive has a thick wall. Negative has a thin wall + outer membrane.
Clinical Impact
Determines antibiotic choice, toxin release (LPS), and disease severity.
Introduction
In the world of microbiology, bacteria are broadly classified based on the Gram stain, a pioneering laboratory technique developed by Hans Christian Gram in 1884. This differential staining method separates bacteria into two dominant categories based on the chemical and physical properties of their cell walls.
Clinical Importance: Knowing whether a bacterium is Gram-positive or Gram-negative is highly critical. It immediately informs a physician about the bacterium’s potential resistance mechanisms, the types of toxins it might release, and which antibiotics will be most effective.
Both bacterial classifications are the primary focus in clinical diagnostics (prescribing empirical therapy), laboratory research (understanding disease pathology), and pharmacology (designing new antimicrobial drugs).
What are Gram-Positive Bacteria?
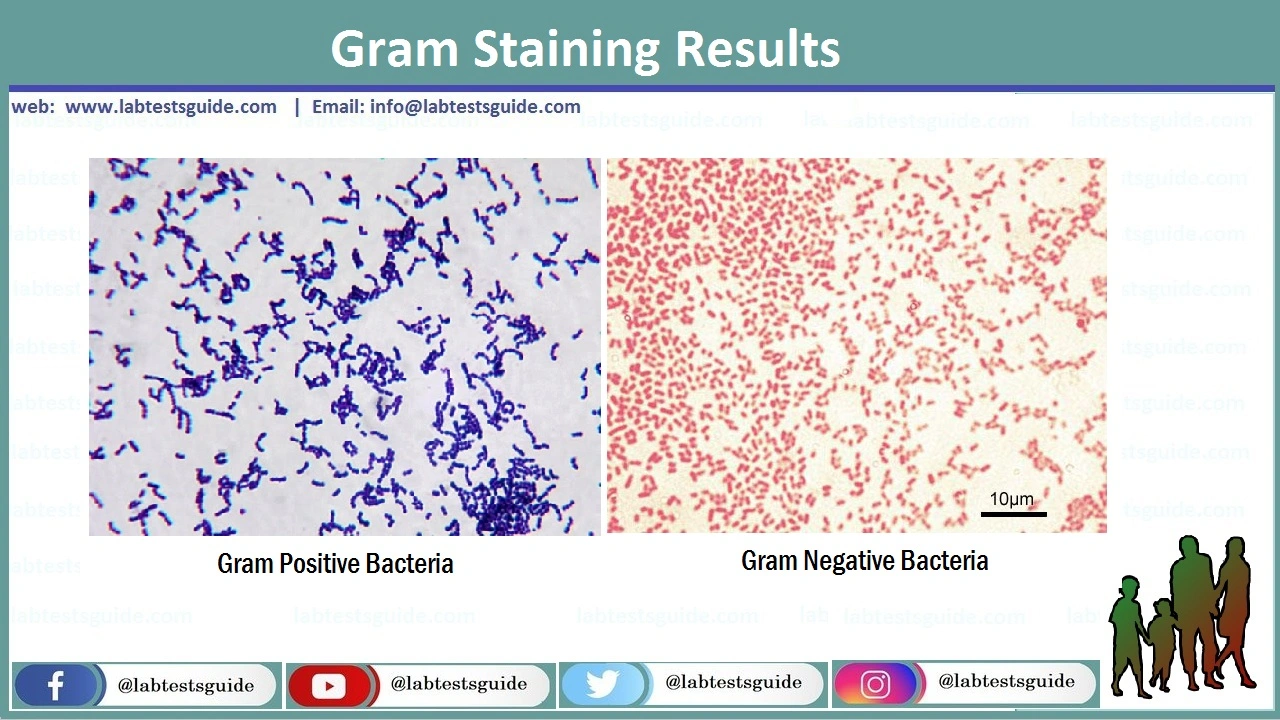
Definition: Gram-positive bacteria are a group of bacteria that retain the primary stain (crystal violet) during the Gram staining procedure, appearing deep purple or blue under a light microscope.
- Key Features: They lack an outer lipid membrane but compensate by possessing a massively thick, robust peptidoglycan cell wall.
- Structure / Composition: The cell wall is up to 90% peptidoglycan (20-80 nm thick). Highly specific to this group are Teichoic acids and Lipoteichoic acids, which act as antigens and help anchor the cell wall to the membrane. Their lipid content is very low (1-4%).
- Function / Role: They function as vital members of the normal human flora (protecting the skin and gut) but can also be highly pathogenic. Many produce powerful exotoxins (e.g., botulinum toxin, tetanus toxin).
- Examples: Staphylococcus aureus, Streptococcus pneumoniae, Bacillus anthracis, and Clostridium tetani.
What are Gram-Negative Bacteria?
Definition: Gram-negative bacteria fail to retain the crystal violet stain after the decolorization step. Instead, they take up the counterstain (safranin) and appear pink or red under a microscope.
- Key Features: Structurally, they are vastly more complex. They possess a thin inner cell wall but are heavily protected by an outer lipid membrane, making them notoriously resistant to many standard antibiotics.
- Structure / Composition: They possess a very thin peptidoglycan layer (only 10% of the wall, 2-8 nm thick) floating in a distinct periplasmic space. The outer membrane contains a high lipid content (11-22%), Porin proteins, and dangerous Lipopolysaccharides (LPS).
- Function / Role: Found commonly in the GI tract and aquatic environments. The LPS layer acts as an endotoxin. When the bacteria die, LPS is released, triggering massive immune reactions that can lead to septic shock.
- Examples: Escherichia coli (E. coli), Salmonella typhi, Pseudomonas aeruginosa, and Neisseria gonorrhoeae.
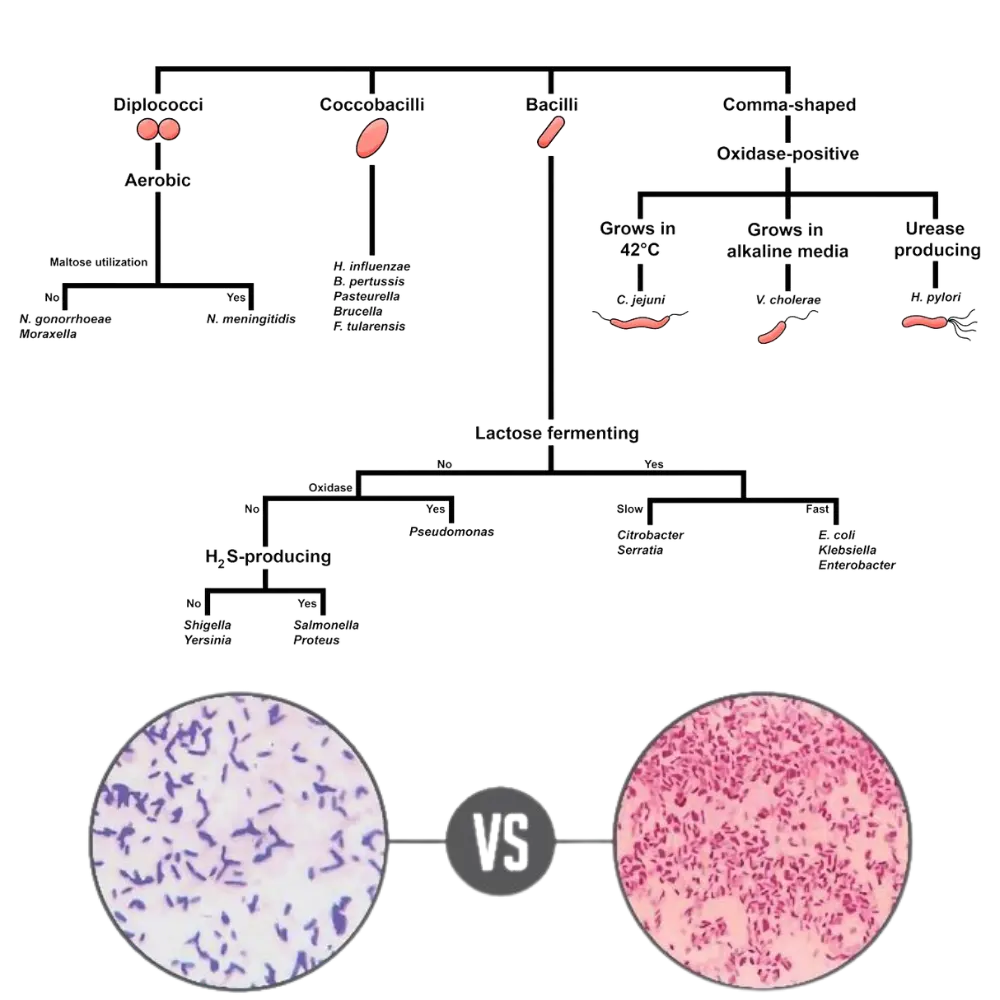
Key Differences: Gram-Positive vs Gram-Negative
Below is a comprehensive, highly detailed 14-point diagnostic comparison for students, researchers, and lab technicians.
| Feature | Gram-Positive Bacteria | Gram-Negative Bacteria |
|---|---|---|
| 1. Gram Stain Color | Retain crystal violet (Appear Purple/Blue) | Take up safranin counterstain (Appear Pink/Red) |
| 2. Peptidoglycan Layer | Very thick, multi-layered (20–80 nm) | Very thin, single-layered (2–8 nm) |
| 3. Outer Membrane | Absent | Present (Acts as a strong barrier) |
| 4. Teichoic Acids | Present (Teichoic & lipoteichoic acids) | Absent |
| 5. Lipopolysaccharide (LPS) | Absent | Present (Functions as an endotoxin) |
| 6. Lipid Content | Very low (1–4%) | High (11–22%) due to the outer membrane |
| 7. Periplasmic Space | Absent or very rare/small | Present and highly distinct (contains enzymes) |
| 8. Porin Proteins | Absent (nutrients diffuse through thick wall) | Present in the outer membrane (controls entry) |
| 9. Flagellar Structure | Basal body has 2 rings (S and M rings) | Basal body has 4 rings (L, P, S, M rings) |
| 10. Toxin Production | Primarily produce Exotoxins | Produce Exotoxins AND Endotoxins (LPS) |
| 11. Susceptibility to Lysozyme | High (Lysozyme easily breaks the thick wall) | Low (Outer membrane protects the thin wall) |
| 12. Antibiotic Resistance | Generally more susceptible (e.g., to Penicillin) | Highly resistant due to outer membrane barrier |
| 13. Physical Disruption | Highly resistant to physical stress/drying | More fragile against physical disruption |
| 14. Examples | Staphylococcus, Streptococcus, Bacillus | E. coli, Salmonella, Pseudomonas |
Similarities Between Both Groups
Despite their vast differences in cell wall anatomy, both groups are fundamentally bacteria and share essential biological traits:
- 1. Prokaryotic Nature: Both completely lack a true membrane-bound nucleus and specialized organelles (like mitochondria).
- 2. Inner Cell Membrane: Both possess a selectively permeable inner phospholipid bilayer (plasma membrane) that regulates ion and nutrient transport.
- 3. Genetic Material: Both contain their genetic information as circular, double-stranded DNA floating in the nucleoid region.
- 4. Ribosomes: Both groups utilize 70S ribosomes (composed of 50S and 30S subunits) for protein synthesis.
- 5. Peptidoglycan Presence: While differing in thickness, both contain peptidoglycan (murein) in their cell walls.
- 6. Plasmids: Both can carry plasmids (extra-chromosomal DNA) which often harbor antibiotic resistance genes.
- 7. Reproduction: Both reproduce asexually through a rapid process called binary fission.
- 8. Motility: Both groups have species that possess flagella for movement.
- 9. Appendages: Both can have pili and fimbriae to assist in attaching to host tissues or transferring DNA.
- 10. Capsule Formation: Species from both groups can develop a protective polysaccharide capsule to evade the host immune system.
- 11. Pathogenicity: Both groups contain severe human pathogens capable of causing opportunistic, community-acquired, and hospital-acquired infections.
Biological Advantages and Disadvantages
Gram-Positive Bacteria
👍 Advantages (Strengths):
- Thick cell wall provides immense protection against physical disruption and osmotic pressure.
- Can survive on dry, inanimate surfaces (like skin, doorknobs) for extended periods.
👎 Disadvantages (Vulnerabilities):
- Lack of an outer membrane makes them highly susceptible to beta-lactam antibiotics (penicillins), lysozyme, and basic detergents.
Gram-Negative Bacteria
👍 Advantages (Strengths):
- Outer lipid membrane naturally blocks large antibiotic molecules, toxic dyes, and harsh detergents.
- Possess highly selective porins that allow nutrients in while keeping chemical threats out.
- Can release endotoxins to severely disrupt host immunity.
👎 Disadvantages (Vulnerabilities):
- Thin peptidoglycan layer makes them prone to physical crushing or mechanical disruption.
- Require damp/moist environments; they die quickly on dry surfaces.
Clinical & Practical Significance
- Diagnostic Importance: The Gram stain is the absolute first step in identifying a bacterial infection in a lab. It allows doctors to begin empirical antibiotic therapy immediately.
- Role in Diseases: Gram-positive infections often present as localized skin abscesses, toxic shock syndrome, or upper respiratory issues. Gram-negative infections frequently involve the gut (gastroenteritis) or urinary tract and carry a high risk of life-threatening endotoxic (septic) shock.
- Lab Usage & Sterility: Differentiating these bacteria is standard protocol in municipal water testing, food safety analysis, and pharmaceutical sterility checks.
When to Suspect Gram-Positive vs Gram-Negative
A rapid decision-making guide for medical scenarios:
🟣 Suspect Gram-Positive when dealing with:
Skin infections (boils, impetigo, cellulitis), throat infections (Strep throat), post-surgical wound infections, and community-acquired pneumonia.
Treatment focus: Cell-wall synthesis inhibitors like Penicillins, Cephalosporins, or Vancomycin.
🔴 Suspect Gram-Negative when dealing with:
Urinary Tract Infections (UTIs), food poisoning (Salmonella), severe intra-abdominal infections, and hospital-acquired ventilator pneumonias.
Treatment focus: Broad-spectrum antibiotics or agents that specifically bypass the outer membrane (like Aminoglycosides or Carbapenems).
Summary Table (Quick Revision)
Short and exam-focused for rapid memorization.
| Point | Gram-Positive | Gram-Negative |
|---|---|---|
| Key Structural Idea | Thick peptidoglycan wall, no outer membrane. | Thin wall, protected by a toxic outer lipid membrane. |
| Unique Identifiers | Contains Teichoic Acid. Stains Purple. | Contains Lipopolysaccharide (LPS). Stains Pink. |
| Clinical Focus | Skin, respiratory, and mucous diagnostics. | GI tract, urinary tract, and aquatic environments. |
| Medical Importance | Easier to treat but highly contagious on dry surfaces. | Harder to treat (antibiotic resistant) & causes sepsis. |
Frequently Asked Questions (FAQs)
What is the main difference between Gram-Positive and Gram-Negative bacteria?
Give some examples of gram-positive bacteria.
Which type of bacteria is generally more dangerous or harder to treat?
Are Teichoic acid and LPS found in both types?
What is more harmful, gram-positive bacteria or gram-negative bacteria?
Why do Gram-positive bacteria stain purple during the lab test?
Is it easier to kill gram-positive bacteria?
What infections are caused by gram-positive bacteria?
What infections are caused by gram-negative bacteria?
Conclusion
In summary, the distinction between Gram-Positive and Gram-Negative bacteria forms the fundamental cornerstone of modern microbiology and infectious disease management. While they share essential cellular machinery, their structural differences drastically alter how they interact with host immune systems and antimicrobial drugs.
💡 Key Takeaway: Gram-positive bacteria rely on a thick peptidoglycan armor and teichoic acids, making them tough against physical elements but vulnerable to basic cell-wall-targeting antibiotics. Conversely, Gram-negative bacteria employ a stealthy, toxic outer membrane loaded with LPS, rendering them highly resistant to medications and representing a complex hurdle in critical medical care.
References:
- Madigan MT, Martinko JM, Bender KS, Buckley DH, Stahl DA. Brock Biology of Microorganisms. 15th edition. Pearson; 2018. (https://www.pearson.com/us/higher-education/product/Madigan-Brock-Biology-of-Microorganisms-15th-Edition/9780134261928.html)
- Tille PM. Bailey and Scott’s Diagnostic Microbiology. 14th edition. Elsevier; 2016. (https://www.elsevier.com/books/bailey-and-scotts-diagnostic-microbiology/tille/978-0-323-35844-2)
- Tortora GJ, Funke BR, Case CL. Microbiology: An Introduction. 13th edition. Pearson; 2019. (https://www.pearson.com/us/higher-education/program/Tortora-Microbiology-An-Introduction-13th-Edition/PGM2267994.html)
- American Society for Microbiology. Gram-Positive and Gram-Negative Bacteria. (https://www.asm.org/Articles/2017/June/Gram-Positive-and-Gram-Negative-Bacteria)
- Centers for Disease Control and Prevention. Identification of Gram-Negative Bacteria. (https://www.cdc.gov/microbiology/ laboratory/gram-negative-bacteria.html)
- World Health Organization. Laboratory Biosafety Manual. 3rd edition. WHO; 2004. (https://www.who.int/publications/i/item/WHO-CDS-CSR-LYO-2004.11)