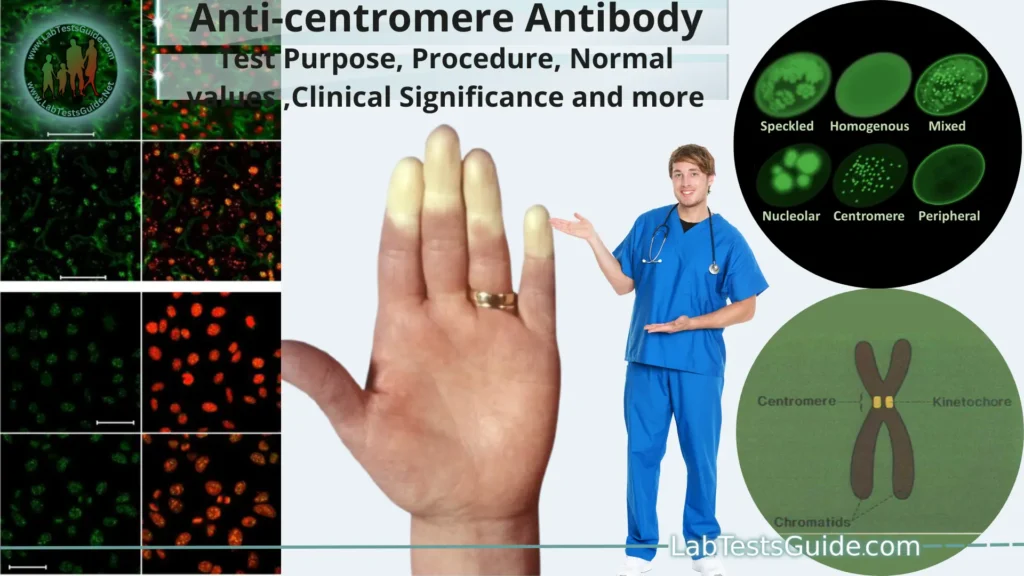
The anti-centromere antibody (ACA) test is a medical laboratory test used to detect the presence of specific antibodies in the blood that target centromere proteins. Centromeres are specialized regions on chromosomes that play a crucial role in cell division and the separation of chromosomes during cell replication.
| Test Name | Anticentromere Antibody |
| Test Purpose | Detect the presence of anti-centromere antibodies; to help diagnose limited cutaneous scleroderma, a subtype of scleroderma |
| Test Preparations | Overnight Fasting Is Preferred. |
| Test Components | ANA Profile, Scleroderma Comprehensive Profile |
| Specimen | 2 ML (1 ML Min.) Serum From 1 SST. Ship Refrigerated Or Frozen. Overnight Fasting Is Preferred. |
| Stability Room | N/a |
| Stability Refrigerated | 72 Hrs |
| Stability Frozen | 2 Weeks |
| Method | Enzyme Immunoassay |
| Download Report | Download Anticentromere Antibody |
Purpose and significance of the test:
The Anticentromere Antibody (ACA) test serves an essential role in diagnosing and understanding certain autoimmune disorders, particularly those associated with CREST syndrome. Here’s the purpose and significance of the ACA test:
Purpose: The primary purpose of the ACA test is to detect the presence of anticentromere antibodies in a person’s blood. These antibodies target specific proteins found in the centromere region of chromosomes, which play a crucial role in cell division and chromosome segregation. The presence of these antibodies is indicative of an immune system response that mistakenly targets the body’s own tissues, leading to autoimmune reactions.
Significance: The significance of the ACA test lies in its ability to aid in the diagnosis and management of autoimmune disorders, specifically those linked to CREST syndrome (Calcinosis, Raynaud’s phenomenon, Esophageal dysfunction, Sclerodactyly, Telangiectasia):
- Diagnosis of Autoimmune Conditions: ACA is strongly associated with CREST syndrome, a subtype of systemic sclerosis (scleroderma). Detecting ACA in a patient’s blood provides valuable information for diagnosing CREST syndrome and distinguishing it from other autoimmune or connective tissue disorders.
- Early Detection and Treatment: Identifying ACA early can allow for timely diagnosis and intervention, enabling healthcare providers to implement appropriate treatment strategies to manage symptoms and potentially slow disease progression.
- Predictive Value: The presence of ACA is often linked to specific clinical manifestations of CREST syndrome, such as Raynaud’s phenomenon, skin changes, and gastrointestinal issues. Testing positive for ACA can help predict the likelihood of developing these symptoms and guide medical monitoring.
- Clinical Management: For individuals diagnosed with CREST syndrome or related autoimmune conditions, ACA testing can aid in determining the severity of the disease and its potential complications. This information is vital for developing personalized treatment plans and providing patients with optimal care.
- Monitoring Disease Progression: Periodic ACA testing can be used to monitor the course of the disease and track changes in antibody levels over time. This helps healthcare providers assess treatment effectiveness and adjust therapies as needed.
- Research and Understanding: ACA testing contributes to a deeper understanding of the immune system’s involvement in autoimmune diseases. It also provides insights into the mechanisms underlying CREST syndrome and related conditions, which can guide further research efforts.
Autoimmune Diseases and Centromere Proteins:
Autoimmune diseases are conditions in which the immune system, which is designed to defend the body against harmful substances, mistakenly attacks and damages its own healthy tissues. Centromere proteins, on the other hand, play a critical role in cell division and chromosome segregation. Understanding the connection between autoimmune diseases and centromere proteins can provide insights into the development of certain autoimmune conditions. Here’s an overview:
Autoimmune Diseases: Autoimmune diseases encompass a wide range of disorders, each with its unique characteristics and affected tissues. In these conditions, the immune system fails to distinguish between self and non-self substances, leading it to produce antibodies that attack and damage normal cells and tissues. Examples of autoimmune diseases include rheumatoid arthritis, lupus, multiple sclerosis, and systemic sclerosis (scleroderma).
Centromere Proteins: Centromeres are specialized regions on chromosomes that play a crucial role in cell division, particularly during mitosis and meiosis. They ensure the accurate separation of chromosomes into daughter cells by forming the attachment point for microtubules of the mitotic spindle. Centromere proteins are essential components of these structures, ensuring proper chromosome segregation and cell division.
Connection and Significance: In the context of autoimmune diseases, centromere proteins gain significance due to the production of specific autoantibodies that target them. One example is the production of anticentromere antibodies (ACAs) that target centromere proteins. These antibodies are associated with a particular subtype of systemic sclerosis known as CREST syndrome:
- CREST Syndrome: CREST syndrome is characterized by the following symptoms: Calcinosis (calcium deposits in the skin), Raynaud’s phenomenon (abnormal blood vessel spasms), Esophageal dysfunction (difficulty swallowing), Sclerodactyly (skin thickening on fingers), and Telangiectasia (dilated blood vessels causing red spots on the skin). ACA presence is highly indicative of CREST syndrome.
- Other Autoimmune Diseases: While ACA is primarily associated with CREST syndrome, the relationship between centromere proteins and other autoimmune diseases is still being explored. Some research suggests that antibodies targeting centromere proteins might be present in other autoimmune conditions, but the significance of these findings varies.
ACA Test Procedure:
The Anticentromere Antibody (ACA) test is a diagnostic procedure used to detect the presence of anticentromere antibodies in a patient’s blood. These antibodies are associated with autoimmune conditions like CREST syndrome. Here’s an overview of the ACA test procedure:
1. Sample Collection:
- A healthcare professional will collect a blood sample from a vein, usually in the arm.
- The blood is drawn into a special blood collection tube (serum separator tube) that helps separate the serum or plasma from the blood cells.
2. Sample Processing:
- After collection, the blood sample is allowed to clot, and then it is centrifuged to separate the serum or plasma from the blood cells.
3. Test Preparation:
- The serum or plasma is carefully prepared to be used in the ACA test. Reagents and test kits specific to the ACA test are used for this purpose.
4. Enzyme-Linked Immunosorbent Assay (ELISA) Method:
- ELISA is a common technique used to detect antibodies in a sample.
- A microplate is coated with centromere antigens (proteins) that react with any anticentromere antibodies present in the sample.
- The processed serum or plasma is added to the microplate wells and allowed to react with the antigens.
5. Detection:
- If anticentromere antibodies are present in the sample, they will bind to the coated antigens on the microplate.
6. Washing:
- The microplate is washed to remove any unbound components.
7. Secondary Antibody Binding:
- A secondary antibody that is linked to an enzyme is added to the microplate. This secondary antibody binds to any bound anticentromere antibodies.
8. Substrate Reaction:
- A substrate is added to the microplate, and if the secondary antibody is bound to the primary antibodies (anticentromere antibodies), an enzymatic reaction occurs, producing a detectable signal.
9. Signal Measurement:
- The intensity of the signal is measured using a spectrophotometer. This measurement correlates with the amount of anticentromere antibodies in the sample.
10. Result Interpretation:
- The test results are interpreted based on the intensity of the signal. The results are reported as positive, negative, or equivocal.
- Positive results indicate the presence of anticentromere antibodies, suggesting a potential autoimmune condition like CREST syndrome.
- Negative results indicate the absence of these antibodies.
11. Clinical Evaluation:
- Test results should be interpreted in the context of the patient’s clinical symptoms, medical history, and other diagnostic tests.
Normal Values of ACA Test:
| Test Result | Interpretation |
|---|---|
| Negative | No detectable ACA antibodies in the blood. |
| Positive | Presence of ACA antibodies in the blood, indicating a potential autoimmune condition such as CREST syndrome. Further evaluation and clinical correlation are needed. |
| Equivocal | Borderline result; requires follow-up testing or additional clinical assessment to determine the significance of the result. |
| Antibody Titer Levels | Positive result with higher levels of antibodies may suggest a stronger association with autoimmune conditions. |
Techniques Used in ACA Test:
The Anticentromere Antibody (ACA) test employs specific laboratory techniques to detect the presence of anticentromere antibodies in a patient’s blood. The most common techniques used for the ACA test are the Enzyme-Linked Immunosorbent Assay (ELISA) and the Indirect Immunofluorescence Assay (IFA). Here’s an overview of both techniques:
1. Enzyme-Linked Immunosorbent Assay (ELISA):
- ELISA is a widely used technique for detecting and quantifying specific antibodies or antigens in a sample.
- Steps involved in ELISA for ACA testing:
- Coating: Microplate wells are coated with centromere antigens, which will capture any ACA antibodies present in the patient’s sample.
- Sample Addition: The patient’s processed serum or plasma sample is added to the wells. If ACA antibodies are present, they will bind to the coated antigens.
- Washing: Unbound components are washed away to remove non-specific interactions.
- Secondary Antibody: A secondary antibody linked to an enzyme is added. This secondary antibody binds specifically to ACA antibodies that have bound to the coated antigens.
- Substrate Reaction: A substrate is added that reacts with the enzyme to produce a measurable signal, often a color change.
- Signal Measurement: The intensity of the signal is measured using a spectrophotometer, and it corresponds to the amount of ACA antibodies in the sample.
2. Indirect Immunofluorescence Assay (IFA):
- IFA is a technique that uses fluorescent-labeled antibodies to detect specific antigens or antibodies in a sample.
- Steps involved in IFA for ACA testing:
- Substrate Preparation: Patient’s serum or plasma sample is added to a slide or well containing cells with centromere antigens.
- Incubation: The sample is allowed to incubate, allowing any ACA antibodies to bind to the centromere antigens on the cells.
- Washing: Unbound components are washed away.
- Fluorescent Secondary Antibody: A secondary antibody labeled with a fluorescent dye is added. This antibody binds to ACA antibodies, if present.
- Fluorescence Detection: When exposed to specific wavelengths of light, the labeled antibodies emit fluorescent signals. The presence of fluorescence indicates the presence of ACA antibodies.
Clinical Significance:
- Diagnosis of CREST Syndrome: ACA presence is strongly associated with CREST syndrome, aiding in the diagnosis of this subtype of systemic sclerosis.
- Early Detection and Intervention: Identifying ACA early enables timely diagnosis and treatment initiation, potentially slowing disease progression.
- Predictive Marker: ACA positivity can predict the development of specific symptoms such as Raynaud’s phenomenon, aiding in patient monitoring.
- Treatment Guidance: ACA testing helps doctors tailor treatment plans for individuals with autoimmune conditions, improving symptom management.
- Disease Monitoring: Periodic ACA testing allows healthcare providers to assess disease progression and adjust treatment strategies accordingly.
- Research and Understanding: ACA testing contributes to understanding autoimmune mechanisms, facilitating research for improved treatments.
- Differential Diagnosis: ACA presence helps differentiate CREST syndrome from other autoimmune or connective tissue disorders.
- Personalized Care: ACA results guide healthcare providers in providing patient-specific care plans for better disease management.
- Prognostic Value: Higher ACA antibody levels may suggest more advanced disease stages, aiding in prognosis determination.
- Collaborative Diagnosis: ACA test results are part of a comprehensive diagnostic approach, combined with patient history, symptoms, and other tests.
Negative Result:
- No ACA Detected: A negative result indicates that no anticentromere antibodies were found in the blood sample.
- Less Likely for CREST Syndrome: In the context of CREST syndrome, a negative result makes the presence of ACA antibodies, which are often associated with this syndrome, less likely.
- Consider Other Diagnoses: While CREST syndrome is less likely, other autoimmune or connective tissue disorders might still be considered as potential diagnoses.
- Clinical Evaluation Needed: Healthcare providers will consider other clinical information and tests to reach a comprehensive diagnosis.
- Potential for Different Autoantibodies: Negative ACA result doesn’t rule out the possibility of other autoimmune antibodies being present.
- Collaborative Diagnosis: A negative result is just one part of the diagnostic puzzle. Collaboration between patients and healthcare providers is crucial for accurate diagnosis.
Positive Result:
- Presence of ACA Antibodies: A positive result indicates the presence of anticentromere antibodies in the blood sample.
- Suggestive of Autoimmune Condition: The presence of ACA antibodies is strongly associated with autoimmune conditions, particularly CREST syndrome.
- Possible CREST Syndrome: A positive result raises the possibility of CREST syndrome (Calcinosis, Raynaud’s phenomenon, Esophageal dysfunction, Sclerodactyly, Telangiectasia).
- Further Clinical Evaluation Needed: A positive result prompts healthcare providers to conduct additional assessments, considering symptoms and medical history.
- Tailored Treatment and Management: Positive results guide doctors in creating personalized treatment plans for autoimmune conditions.
- Severity Indication: Higher levels of ACA antibodies may correlate with disease severity, aiding in prognosis determination.
- Diagnostic Marker: ACA antibodies provide a valuable diagnostic marker for autoimmune disorders, assisting in distinguishing CREST syndrome from other conditions.
- Collaborative Diagnosis: Positive ACA results are part of a comprehensive diagnostic approach, combined with other clinical information and tests.
FAQs:
Q1: What is the Anticentromere Antibody (ACA) test?
A1: The ACA test is a diagnostic procedure that detects the presence of anticentromere antibodies in a blood sample. These antibodies are associated with autoimmune conditions like CREST syndrome.
Q2: What is CREST syndrome?
A2: CREST syndrome is a subtype of systemic sclerosis characterized by Calcinosis, Raynaud’s phenomenon, Esophageal dysfunction, Sclerodactyly, and Telangiectasia. ACA antibodies are closely linked to CREST syndrome.
Q3: How is the ACA test performed?
A3: The ACA test is usually performed using techniques like Enzyme-Linked Immunosorbent Assay (ELISA) or Indirect Immunofluorescence Assay (IFA). Blood is collected, processed, and analyzed for the presence of ACA antibodies.
Q4: Is fasting required before the ACA test?
A4: In most cases, fasting is not required for the ACA test. However, follow any specific instructions provided by your healthcare provider.
Q5: What does a positive ACA test result mean?
A5: A positive result suggests the presence of ACA antibodies in your blood, indicating a potential autoimmune condition like CREST syndrome. Further evaluation and clinical correlation are needed.
Q6: What does a negative ACA test result mean?
A6: A negative result means that no detectable ACA antibodies were found in your blood sample. While it makes CREST syndrome less likely, clinical assessment and consideration of other factors are important.
Q7: Can a positive ACA result confirm CREST syndrome?
A7: A positive result is indicative of ACA antibodies and suggests a potential link to autoimmune conditions like CREST syndrome. However, it’s part of a diagnostic puzzle and requires further evaluation for confirmation.
Q8: What should I do after receiving ACA test results?
A8: If you receive positive or equivocal results, consult your healthcare provider for further evaluation and guidance. Negative results should also be discussed in the context of your symptoms and medical history.
Q9: Can ACA testing be used for disease monitoring?
A9: Yes, ACA testing can be used to monitor disease progression and treatment effectiveness in individuals diagnosed with CREST syndrome or related autoimmune conditions.
Q10: Are there other tests used in conjunction with ACA testing?
A10: Yes, ACA testing is often part of a comprehensive approach that includes patient history, physical examination, and potentially other tests to arrive at an accurate diagnosis.
Conclusion:
In conclusion, the Anticentromere Antibody (ACA) test holds significant diagnostic value in identifying autoimmune conditions, particularly CREST syndrome. The presence of ACA antibodies indicates potential immune system dysfunction and suggests the need for further clinical assessment. Positive results guide tailored treatment strategies, while negative results prompt consideration of alternative diagnoses. Collaborative interpretation between healthcare providers and patients remains paramount in navigating the complexities of autoimmune disorders and ensuring optimal care.



One Comment